Content
- General characteristics of the disease
- Reasons for the appearance
- Pathogenesis
- Symptoms and Signs
- Infectious or not to others
- Disease classification
- Fresh (soft focal)
- Chronic (fibrous-focal)
- The clinical picture of development: phases
- Diagnostic methods
- X-ray
- Additional research
- Basic principles of therapy
- Drug treatment
- Features of the patient's nutrition
- Recovery prognosis
- Rehabilitation and restoration of the body
- Complications and possible consequences of focal pulmonary tuberculosis
- Disease prevention
- In adults
- In children
Focal pulmonary tuberculosis is a secondary period of the disease that develops in people who have undergone the primary form of a specific infection several years ago. The pathological process proceeds without pronounced symptoms and is more often detected during preventive fluorographic examinations.
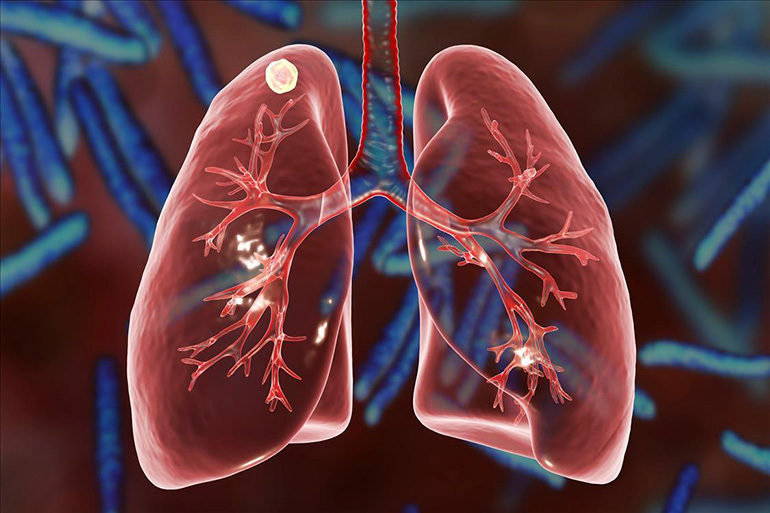
General characteristics of the disease
Focal tuberculosis is referred to as small forms of respiratory tuberculosis. Limited destructive changes are small in size - up to 1 cm in diameter. The disease is diagnosed in 15-20% of patients who have had primary tuberculosis.
Reasons for the appearance
The secondary period of the disease occurs with a decrease in acquired immunity against the background of stress or concomitant diseases: diabetes mellitus, gastric ulcer, pneumoconiosis, HIV infection.
Sometimes the process begins to develop after a course of treatment with immunosuppressants or corticosteroid drugs, which depress the human immune system.
The reintroduction of virulent mycobacteria (exogenous superinfection) may play a decisive role. Such infection occurs through close contact with patients with an open form of tuberculosis.
Another way is endogenous reactivation of residual primary foci in the lungs or in the intrathoracic lymph nodes. The activation of the process is facilitated by prolonged overwork, bad habits (use of alcohol, drugs, smoking), deterioration of nutrition and social conditions.
Pathogenesis
The extent of pathological changes in the lungs depends on the general condition of the body and the ability of the immune system to adequately respond to an exacerbation of the disease. The advantage of the upper lobe localization of foci is determined by various factors:
- insufficient aeration and low mobility of the upper parts of the lungs;
- reduced blood flow and lymph movement;
- a high degree of sensitization, contributing to the fixation of mycobacteria.
Destructive areas are often located in the area of the upper lobe of the right lung, sometimes there is a bilateral process.
Symptoms and Signs
The clinical course of the secondary period of the disease can be manifested by mild symptoms of intoxication. Patients note the following violations:
- deterioration in sleep and appetite;
- general weakness, moderate sweating;
- subfebrile condition (more often in the evening);
- short-term feeling of heat or chills.
Specific intoxication sometimes has signs of hyperthyroidism: enlargement of the thyroid gland, increased heart rate, irritability, weight loss, and menstrual irregularities in women.
Some patients report pain in the flank, interscapular region, or shoulder, dry cough, and small amounts of mucous sputum.
Infectious or not to others
The activation of pathological foci may be accompanied by the growth of bacterial flora and the release of tuberculous mycobacteria into the environment.
Bacilli can be transmitted in a variety of ways:
- Airborne droplets (most common). The infection is transmitted directly from the patient by talking, coughing or sneezing. Communication in closed rooms is especially dangerous.
- Air-dusty. Dried sputum particles, mixing with dust, are lifted into the air with the wind and can enter the nasopharynx of a child or adult.
- Contact and household. In rare cases, infection occurs through the conjunctiva of the eyes or skin in violation of the rules of personal hygiene.
- Intrauterine. Infection from a sick mother to the fetus through the placenta or during childbirth is extremely rare.
In some cases, bacterial excretion is not observed or is scarce.
Disease classification
Focal pulmonary tuberculosis occurs in different forms, which are classified according to the degree and duration of the process, as well as the location and number of foci. By the number of destructive areas, 2 types are distinguished: with a single focus and multiple (2 or more, not related to each other).
Important information: The clinical picture of the course of fibrocavernous pulmonary tuberculosis
By localization of the pathological process, the following forms are diagnosed:
- upper lobe;
- lower lobe;
- middle lobe (in the right lung).
Depending on the duration of the course, the disease can be fresh or chronic.
Fresh (soft focal)
The initial stage of the secondary period is characterized by lesions of the segmental bronchi area. In this case, endo- or peribronchitis is more often detected. When the pulmonary alveoli are involved in the pathological process, lobular bronchopneumonia develops.
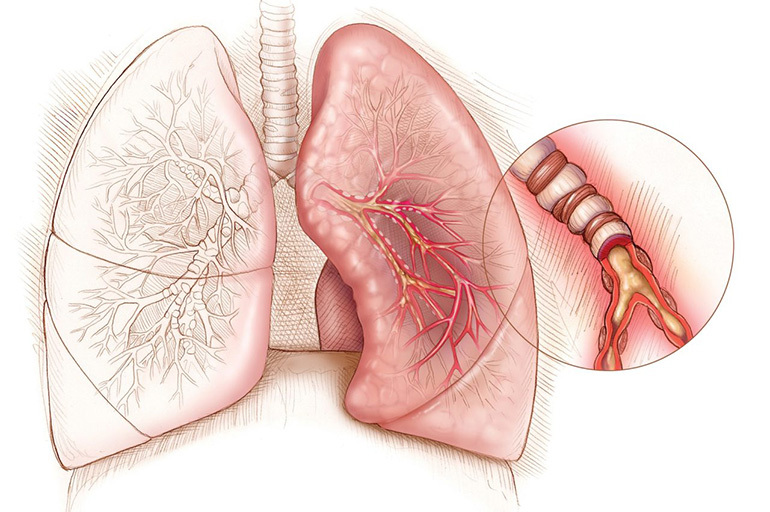
Chronic (fibrous-focal)
The late stage of the disease is characterized by the development of fibrous focal tuberculosis. With resorption of the focus, limited replacement by connective tissue, calcification, encapsulation occurs. The chronic form can be the outcome of fresh mild-focal tuberculosis or other pulmonary forms (infiltrative, disseminated, cavernous).
The clinical picture of development: phases
The development of focal tuberculosis is divided into 3 phases:
- Infiltration - small pathological foci are formed.
- Decay - particles of the affected tissue are excreted by the lungs and bronchioles.
- Seals - foci of fibrosis and calcifications are formed.
In the second phase, the process of melting of cavernous areas and the formation of cavities takes place. At this time, wheezing occurs in the bronchi, moderate hemoptysis appears. In the phase of compaction, the inflammation subsides, the caseoses become denser and are limited to the connective tissue.
The sizes of the foci are small (up to 3 mm in diameter), medium (up to 6 mm) and large (up to 10 mm). The blurring of the clinical picture is explained by the fact that the inflammatory process does not develop actively. In this case, bacterial intoxication has a negative effect on the body.
Diagnostic methods
Focal tuberculosis is detected in various ways. First of all, the doctor examines the patient's history and complaints. On examination, palpation and auscultation, wheezing is sometimes heard (after coughing).
Then other methods are connected, of which the most informative is X-ray examination.
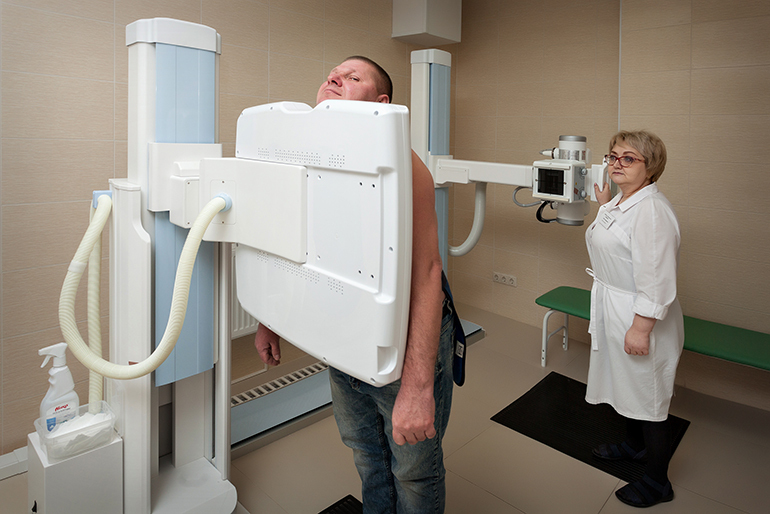
X-ray
On the pictures, which are performed in 2 projections, the syndrome of focal shadows is determined. The picture of soft-focal tuberculosis with indistinct contours of the zone of inflammation differs from fibrous-focal tuberculosis with fibrous cords and impregnations of elements of calcium salts.
Important information: Features of the treatment of different forms of disseminated pulmonary tuberculosis
Differential diagnosis is carried out with pneumonia, pulmonary fibrosis, peripheral tumors and parasitic cysts in the early stages of development.
Additional research
Objective research reveals nonspecific changes:
- muffling percussion sound over the hearth;
- soreness or stiffness in the muscles of the shoulder girdle;
- hard breathing and small bubbling rales on auscultation;
- heart palpitations, high or low blood pressure.
The lymph nodes are normal.
Bronchoscopy with biopsy helps to assess the state of the respiratory system, detect pathogenic microflora, as well as tissue changes. Mycobacteria are found in biomaterials at the stage of decay and cavity formation.
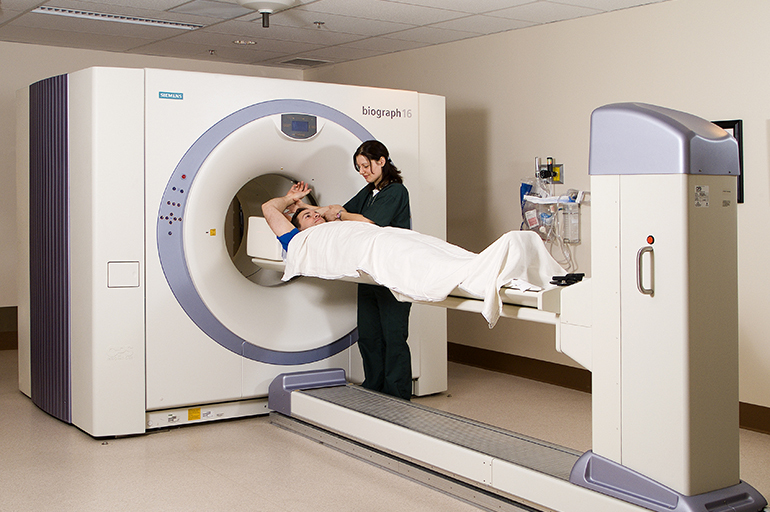
Computed tomography allows you to determine the size, structure and shape of the lesions.
To clarify the diagnosis, sputum analysis for CD is performed (three times with an interval of 14 days), as well as immunological blood reactions (quantiferon test, T-Spot. TB).
A blood test may show an increase in ESR and an increased concentration of stab neutrophils.
Diaskintest and Mantoux test for focal tuberculosis are normal and do not play a decisive role in diagnosis. A positive reaction often indicates the presence of primary tuberculosis.
Basic principles of therapy
Treatment of patients with active tuberculosis is carried out in stationary conditions for 2-3 months. Outpatient therapy lasts 4-6 months.
Comprehensive treatment includes taking anti-tuberculosis, immunomodulating and general strengthening agents.
Physiotherapy procedures help relieve pain, increase sputum discharge, improve blood circulation and tissue regeneration.
Surgical intervention (removal of the affected lobe of the lung) is used in rare cases with the ineffectiveness of antibiotic therapy, frequent relapses with bacterial excretion.
Drug treatment
Chemotherapy standards in the intensive phase include a combination of 3-4 drugs. Anti-tuberculosis drugs such as isoniazid, rifampicin, ethambutol, pyrazinamide are used. At the initial stage, streptomycin may be prescribed.
In the continuation phase of therapy, the combination is reduced to 2 drugs (for example, isoniazid with ethambutol or rifampicin).
Hepatoprotectors are used to protect the liver. Vitamins A, B1, B2 help to strengthen the patient's body. The course of therapy is selected individually by the phthisiatrician.
The result of treatment directly depends on the timeliness of the patient's request for medical help.
Features of the patient's nutrition
The diet of a patient with tuberculosis is one of the components of complex therapy. A therapeutic diet should comply with the main principles:
- The inclusion of protein-rich dishes on the menu.
- Adequate (but moderate) fat intake.
- The predominant use of products containing complex carbohydrates.
- Eating a lot of vegetables and fruits.
It is recommended to use lean meat (beef, pork, rabbit, poultry) as the main supplier of protein (at least 120 g per day). Fish (preferably seafood) and seafood are useful. Every day, the menu includes eggs and dairy products (cottage cheese, sour cream, yogurt, kefir, natural yogurt).

Fresh fruits and vegetables rich in vitamins and fiber should be consumed regularly. It is important to take into account the state of the gastrointestinal tract. In winter, pickled vegetables (different types and varieties of cabbage, bell peppers, eggplants, tomatoes) can be a source of vitamins and microelements.
Important information: Clinical picture and nuances of the development of infiltrative pulmonary tuberculosis
It is recommended to add vegetable fats (unrefined sunflower, olive, corn, linseed or nut oil) to food. Fish oil is useful.
Carbohydrates are essential as a source of energy. For soups and side dishes, it is better to use buckwheat, oatmeal, wheat, pearl barley or rice.
The menu is made at the rate of 5-6 meals a day with intermediate snacks in the form of fruit drinks, fresh berries and fruits, nuts, sunflower seeds or pumpkin.
Recovery prognosis
A favorable outcome of the disease is ensured not only by timely and competent treatment, but also by the patient's adequate behavior. It is important to strictly follow the doctor's recommendations, observing the regime and rules of hygiene.
A long course of treatment (6-12 months) promotes the resorption of pathological foci and the restoration of the body.
Recovery without consequences and complications occurs in most cases.
Rehabilitation and restoration of the body
After completing the course of treatment, all patients are recommended rehabilitation in an anti-tuberculosis sanatorium. Dispensary observation by a phthisiatrician lasts 1.5-2 years after recovery. In the spring and autumn, a prophylactic course of anti-tuberculosis drugs is prescribed.

Fluorography or X-ray examination is performed annually (sometimes 2 times a year).
It is necessary to constantly observe the mode of work and rest, avoid infectious and colds, and provide adequate nutrition.
Complications and possible consequences of focal pulmonary tuberculosis
Launched and untreated forms of focal tuberculosis can give the following complications:
- pleurisy;
- pneumothorax;
- pulmonary bleeding;
- medicinal hepatitis;
- infiltrative tuberculosis;
- cavernous tuberculosis;
- the formation of cavernous capsules more than 1 cm in diameter.
Untimely treatment and extreme weakening of the body can be fatal.
MMM
Disease prevention
Specialized centers and other treatment-and-prophylactic institutions are engaged in the prevention of outbreaks of tuberculosis among the population.
In adults
Annual fluorographic examination is recommended from the age of 18. In the presence of a predisposition to pulmonary diseases, work in hazardous conditions or suspicion of contact with a patient with tuberculosis, open examinations are carried out more often.
In children
Specific anti-tuberculosis prophylaxis is carried out in the first days of a newborn's life. BCG vaccination contributes to the formation of strong immunity in a child. Revaccination is done at 6-7 years after a negative Mantoux test.
Non-specific prevention is about adhering to the principles of a healthy lifestyle. The child needs walks in the fresh air, exercise, balanced nutrition, healthy sleep, positive emotions. It is important to maintain personal hygiene and keep your home clean.



