- the presence of blood in the feces on only one side (where the crack is located);
- acute pain during bowel movement and within 10 - 15 minutes. after defecation - going to the toilet becomes painful;
- spasm of the sphincter of the rectum.
The chronic form of the disease has been present for a long time (more than 30 days). With this type, the edges of the crack are curved, there is a deposit at the bottom. Long-term pain is distinguished as symptoms. Moreover, the discomfort becomes stronger not only after emptying the intestines, but also when the body is in one position for a long time. A person begins to be afraid of going to the toilet, takes laxatives to facilitate bowel movements. Additionally, pus may form in the cracks (a running process).
The chronic form is subdivided into an exacerbation or remission phase. In the first case, the symptoms of the disease appear vividly. Remission (lasts from 20 days) is a fading away of symptoms, that is, it seems to the person that they managed to get rid of the crack.
Acute defects heal in 40-60% of people when the stool returns to normal. If this does not happen, the crack can degenerate into a chronic form.
- anemia;
- dehydration;
- impaired blood formation;
- bleeding;
- diseases of the urinary organs;
- oncology;
- reduced protective functions of the body;
- blood poisoning;
- allergic reaction.
Preparatory measures:
1. It is not recommended to take antibacterial agents 14 days before the KLA (Amoxicillin, Klacid, Sumamed).
2. Alcoholic drinks must be excluded 3 days before the study.
3. Exclude physical activity in 24 hours.
4. Do not smoke 2 - 3 hours before the KLA.
It is better to donate blood on an empty stomach. In the morning, you should not drink coffee and tea, as the result may be distorted. Pure water is not prohibited. If the collection of biomaterial is carried out in the afternoon, a light breakfast is allowed 4 hours before the study.
Blood can be drawn from a vein or from a finger. Some private laboratories only use the first view, as the result is more accurate. The term for the study of the biomaterial is from 1 to 3 days.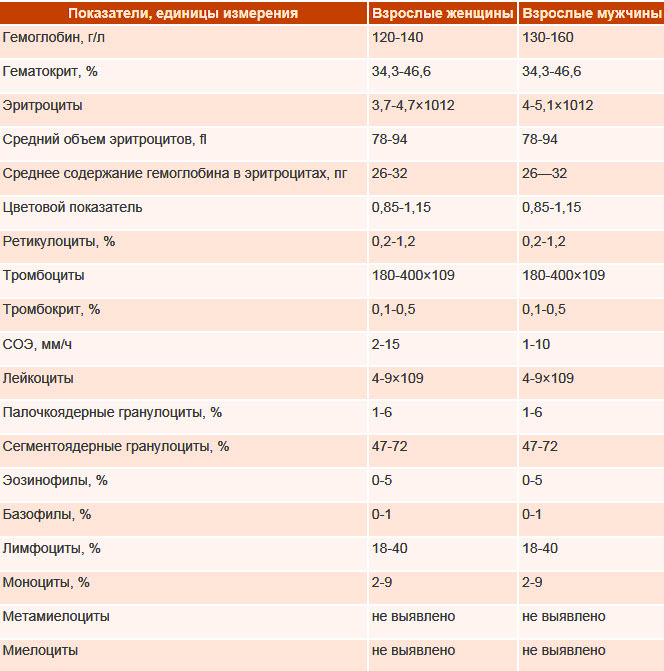
1. It is not recommended to take medications for 7 days.
2. Cystoscopy (examination of the bladder) should not be performed 5 to 7 days before OAM.
3. 2 days before urine collection, exclude alcohol.
4. 24 hours before collecting the biomaterial, exclude foods that can stain urine (bright fruits and vegetables), as well as sweet, smoked foods.
5. Exclude physical activity 24 hours before OAM.
6. 12 hours before urine collection, you should refuse contact with a partner.
Before collecting biomaterials, it is recommended to purchase a container at a pharmacy. If this is not possible, replacement with a can with a volume of up to 200 ml is allowed. It is treated with soapy water, poured over with boiling water, and dried. Biomaterial collection rules:
1. Wash off with warm water and baby soap.
2. Open the urine container.
3. Collect the morning urine that accumulates at night. Let some liquid out into the toilet, without stopping the process, fill the container with biomaterial.
4. Close the container carefully.
The container with biomaterial must be delivered to the laboratory within 1 - 2 hours. The analysis is ready for 1 to 3 days.
1. For 7 days, exclude the use of drugs that affect intestinal motility. For example, laxatives (Guttalax, Senade, Duphalac), sorbents (Filtrum-STI, Lactofiltrum, Enterosgel), iron products (Ferretab, Ferrum Lek, Totema). It is also recommended to abandon the use of antidiarrheal drugs (Loperamide, Imodium) and medicines, which include components that change the color of feces (bismuth, barium and others). Additionally, antibacterial agents should not be taken, as they disrupt the intestinal microflora.
2. If it is necessary to reveal occult blood, then 3 - 5 days before the study, it is recommended to exclude protein products (meat, eggs, etc.).
3. At least 3 days in advance, exclude products that can affect the color of the biomaterial (beets, carrots, etc.). Additionally, it is recommended to give up fatty, fried, smoked products. Coloring, carbonated drinks are prohibited.
4. For 1 - 2 days, exclude the use of rectal suppositories and cleansing enemas. Additionally, it is not recommended to undergo diagnostic procedures that irritate the anus and rectum (sigmoidoscopy, colonoscopy).
5. Exclude contacts with a sexual partner within 24 hours.
Women are not recommended to perform a coprogram during menstruation, as discharge can distort the study. But if the result is needed urgently, the doctor prescribes an analysis. In this case, it is recommended to close the entrance to the vagina with a tampon or cotton wool, then empty the intestines and collect the feces in a container.
It is more convenient to place the biomaterial in a sterile container, which is sold in a pharmacy. If this is not possible, you can use any glass jar with a volume of up to 200 ml. Before use, thoroughly wash the container with water and detergent, then rinse with boiling water and dry. The pharmacy container does not need to be processed, it is sterile. Stages of collecting biomaterial:
1. Empty the bladder. If you neglect this point, urine can get into the feces.
2. Wash off with warm water and baby soap, wipe dry.
3. Empty the intestines into a container (bowl or saucepan). It is necessary to wash the container in advance and pour over it with boiling water. It is not recommended to collect feces from the toilet, as microorganisms can get into the biomaterial and the test result will be incorrect.
4. Collect feces with a spoon or wooden stick. Place the masses in a container or jar. For analysis, 1 tsp is enough. biomaterial. But it is better to collect a sample from different parts of the feces. For example, from the top, collecting, from the middle of the feces.
5. Place the container with feces in the refrigerator. The biomaterial must be delivered to the laboratory within 10 hours from the moment of collection.
The term for the study of the biomaterial is from 1 to 3 days. The following data is indicated in the result sheet:
- consistency;
- Colour;
- smell;
- the presence of undigested food;
- the presence of mucus;
- the presence of pus;
- worms or their eggs;
- pH (acidity);
- hidden blood;
- microscopic parameters (ammonia, starch and others).
- exclude fatty, fried, smoked foods for 3 days, since foods can lead to excessive gas formation;
- use laxatives or a cleansing enema (in the evening before the procedure and in the morning before anoscopy);
In the morning it is better to carry out anoscopy on an empty stomach. But if the research is done in the afternoon, a light breakfast is allowed.
Anoscopy can be performed in three positions:
- the patient gets on all fours and rests on his elbows;
- the person lies on his back;
- the patient lies on his left side, bends the lower limbs at the knees and pulls them to the chest.
Stages of the procedure:
1. The health worker puts on gloves, covers them with anesthetic.
2. The rectum is palpated. That is, the doctor inserts his finger into the anus.
3. An anoscope is taken, which is equipped with a light element. The device is a smooth rod up to 1 cm in diameter. The tip of the device is moistened with medication or oil and moves into the anus, an examination is carried out.
4. The anoscope is removed from the rectum.
The procedure takes no more than 20 minutes. The examination may take a tissue sample for biopsy or remove a polyp.
There is another type of procedure - videoanoscopy. A camera is built into the device, and the image is displayed on the monitor in real time. Additionally, it is possible to record the procedure.
Rectoromanoscope is a tube with a diameter of no more than 20 mm. At the end of the device there is an optical system (lenses and glasses), and inside there is a light element.
With sigmoidoscopy, it is possible to remove a polyp or neoplasm, take a tissue sample for biopsy. Additionally, it is allowed to stop bleeding, expand the anal canal (if it is narrowed).
Preparatory measures:
1. For 2 days, exclude products that can cause fermentation. For example, soda, fruits and vegetables. It is also not recommended to drink alcohol. Additionally, you need to give up fatty, flour, sweet.
2. Clean the intestines twice with an enema or laxative - in the evening before the study and in the morning before rectoscopy.
Stages of the procedure:
1. The patient is asked to lie on a couch, bend the lower limbs at the knees and press them against the chest. But another position is possible - a person gets on all fours and rests on his elbows.
2. The tip of the device is lubricated with a product, the device is inserted into the anus. To facilitate the process, the person may be asked to strain.
3. The device that cuts off the air supply is removed from the tube.
4. Air is pumped. This is necessary to straighten the intestinal walls and improve visualization.
5. The tube is gradually advanced along the rectum.
6. If necessary, after the examination, additional procedures are performed (removal of the polyp, tissue sampling for biopsy, etc.).
7. Air is discharged from the intestine, the apparatus is extracted from the rectum.
The duration of the procedure does not exceed 15 minutes. If rectoscopy is performed on children, general anesthesia may be administered.