Content
- Principle and mechanism of action of B-lactam antibiotics, resistance
- Indications for use, antimicrobial activity
- Contraindications
- Side effects and overdose
- Overdose
- Classification and description of drugs in the group
- Natural penicillins
- Benzylpenicillin
- Phenoxymethylpenicillin
- Penicillin-susceptible penicillins
- Oxacillin
- Cloxacillin
- Aminopenicillins
- Ampicillin
- Amoxicillin
- Carboxypenicillins
- Carbenicillin
- Ureidopenicillins
- Azlocillin
- Inhibitor-protected penicillins
- Amoxicillin / clavulanate
- Ampicillin / sulbactam
- Amoxicillin / sulbactam
- Ticarcillin / clavulanate
- Cephalosporins
- Generation I cephalosporins
- Generation II cephalosporins
- Generation III cephalosporins
- Generation IV cephalosporins
- Names and prices of drugs
- Beta-lactams videos
B-lactam antibiotics - it is a group of antibacterial drugs, which are characterized by the obligatory presence of a nitrogen-containing b-lactam ring in the structure. Historically, the first antibiotic (benzylpenicillin) belongs to this class of drugs. It was isolated by microbiologist Alexander Fleming in 1928. And already from the middle of the XX century it began to be used in clinical practice for the treatment of infectious diseases.
Principle and mechanism of action of B-lactam antibiotics, resistance
B-lactam antibiotics have a bactericidal effect. This means that under the influence of these substances, infectious agents die and are excreted from the body. The basic principle of functioning is a violation of the formation of the bacterial cell wall.
The target of action for b-lactams in a microbial cell is carboxy- and transpeptidase enzymes (penicillin-binding proteins). These enzymes are involved in the synthesis of the main component of the cell wall - peptidoglycan murein. This substance, the special structure of which, ensures the strength of the bacterial walls. The peptidoglycan layer is well represented in the cells of gram-positive microorganisms.
The combination of b-lactams with penicillin-binding proteins leads to dysfunction of the latter. As a result, the process of creating cell walls stops, and bacteria die. 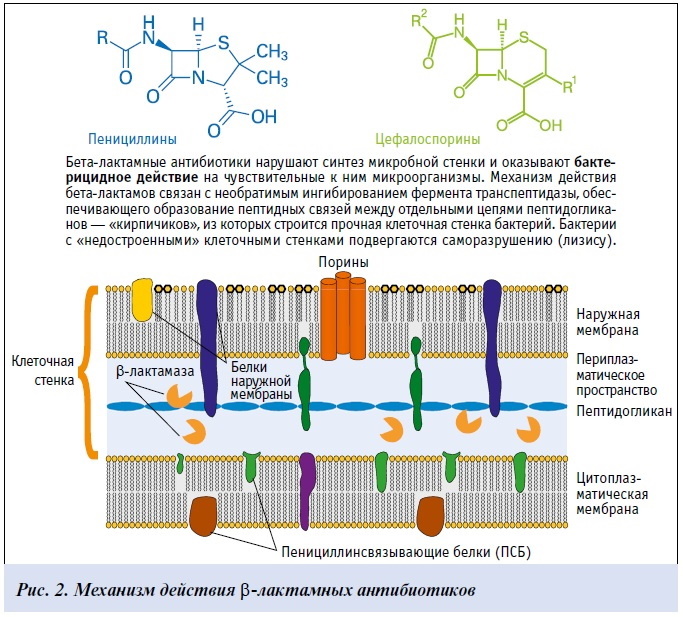
Mechanisms of development of resistance:
- In gram-negative microorganisms, the peptidoglycan layer is weakly expressed. The supporting function in such bacteria is performed by an additional lipid membrane. Most b-lactams penetrate poorly through this membrane. Therefore, gram-negative microbes are relatively resistant to the action of this group of antibiotics.
- Natural or acquired ability of bacteria to produce b-lactamases. These are enzymes that are capable of destroying the structure of b-lactam antibiotics.
- Changes in the structure of penicillin-binding proteins. This mechanism determines the resistance of Staphylococcus aureus and some pneumococci to b-lactams.
Indications for use, antimicrobial activity
B-lactam antibiotics are the basis of modern antimicrobial therapy, since they are characterized by a wide spectrum of activity. B-lactams are highly effective against gram-positive bacteria (except for monobactams), destructive affect gram-negative cocci (Moraxella, Neisseria) and a number of gram-negative rods (Echerihia coli, Proteus mirabilis, Salmonella spp.).
Non-fermenting bacteria and anaerobes are microbes that are naturally resistant to many b-lactams. This fact is explained by the weak permeability of their cell walls and the production of special protective enzymes (b-lactamases).
Infections caused by intracellular bacteria are characterized by resistance to b-lactams, which is associated with the inability of these chemotherapy drugs to penetrate the human immune cells, where the data is microorganisms.
General indications for use:
- Empirical and etiotropic therapy of focal or generalized infection in the body.
- Antibiotic prophylaxis after surgery.
- Prevention of acute rheumatic fever, chronic rheumatic heart disease and glomerulonephritis.
B-lactam antibiotics are drugs that are approved for use during pregnancy and breastfeeding with rare exceptions.
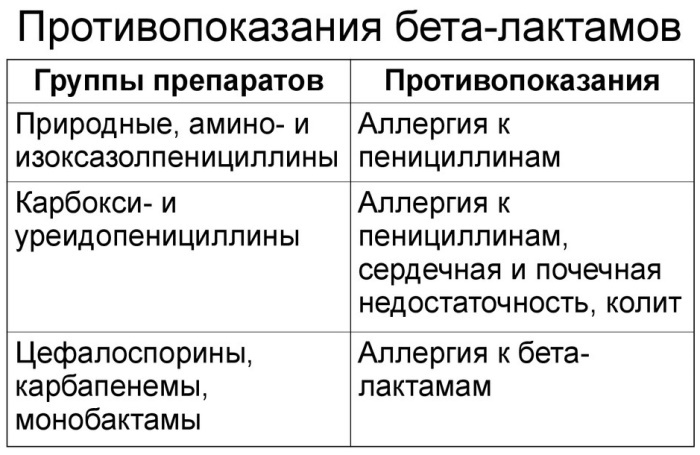
Contraindications
B-lactam antibiotics have a number of restrictions on their use.
These include:
- history of hypersensitivity and allergic reactions to drugs in this group;
- pseudomembranous colitis;
- infectious mononucleosis, lymphoproliferative processes (for ampicillin);
- history of cholestatic jaundice or liver dysfunction (for amoxicillin / clavulanic acid);
- pregnancy (for carbenicillin);
- severe renal dysfunction (for carbenicillin);
- newborns (risk of kernicterus for ceftriaxone).
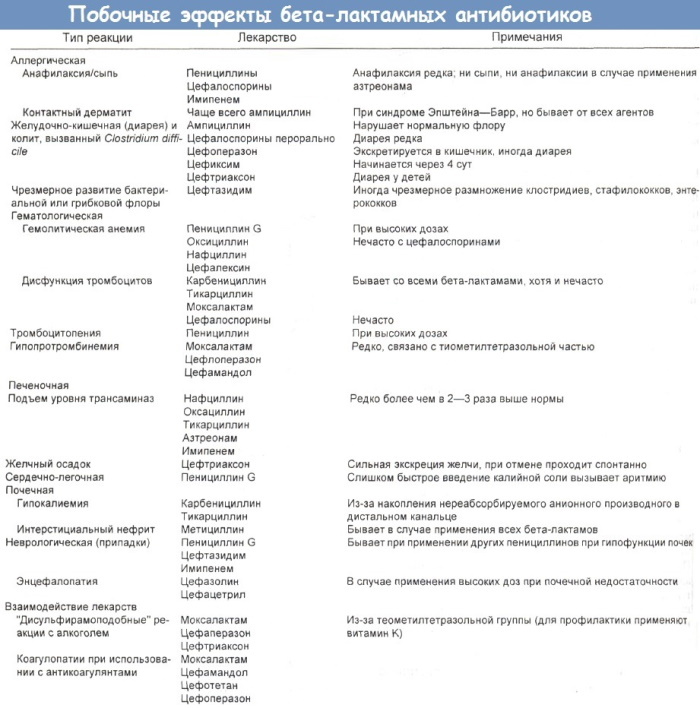
Side effects and overdose
B-lactam antibiotics are the lowest toxic chemotherapy drugs for the human body.
However, a certain number of patients are at risk of developing a number of side effects of a general and local nature:
- Allergic reactions. Allergic reactions can occur if a person has previously taken any of the drugs in this group, since there is a possibility of cross-allergy. The risk of developing hypersensitivity to penicillins is higher than to other representatives of b-lactams. More often, skin manifestations of allergies occur: rashes and swelling, accompanied by itching (urticaria). Less commonly, severe forms: bronchospasm, angioedema or anaphylactic shock.
- Gastrointestinal symptoms. The nonselective effect of b-lactams disrupts the natural intestinal microflora, which can be manifested by the development of antibiotic-associated diarrhea. Also, for all representatives, the appearance of dyspeptic symptoms (nausea, vomiting, pain in the abdomen) is possible.
- Nephrotoxicity. Renal dysfunction may occur with oxacillin.
- Hepatotoxicity. A temporary increase in the level of liver enzymes is periodically observed when using b-lactams. This condition stops on its own and does not require special treatment. Cases of hepatitis and cholestatic jaundice have been reported with the use of protected penicillins.
- Hematological reactions. Some cephalosporins and carboxypenicillins can cause the development of hemorrhagic syndrome (petechiae on the conjunctiva and mucous membranes, bruising, bleeding).
- Candidiasis. All b-lactams are capable of disrupting the balance of microflora in the organs of the gastrointestinal tract and the genitourinary system. As a result, candidiasis of the oral cavity, esophagus, vagina in women and the penis in men can occur.
- Nervous system symptoms. Headaches, gait coordination problems, anxiety, and confusion may occur.
- Skin manifestations. Rare side effects include severe skin reactions such as erythema multiforme, toxic epidermal necrolysis, and exfoliative dermatitis.

- Local reactions. With intramuscular use, the formation of an infiltrate at the injection site is possible, with intravenous use - the development of thrombophlebitis.
Overdose
With an overdose of b-lactams, a number of symptoms from the digestive tract occur:
- excruciating nausea;
- indomitable vomiting;
- epigastric pain;
- diarrhea.
Violations of the water-electrolyte balance are also observed. Crystalluria is possible with the development of renal dysfunction. With severe concomitant pathology, impaired consciousness and convulsive syndrome occur. There is no specific treatment. Therapy is symptomatic. They monitor vital indicators of gas and water-salt metabolism. The use of hemodialysis is possible.
Classification and description of drugs in the group
B-lactam antibiotics are a collection of drug groups, which include:
- penicillins;
- cephalosporins;
- carbapenems;
- monobactams.
Penicillins are divided into natural and semi-synthetic.
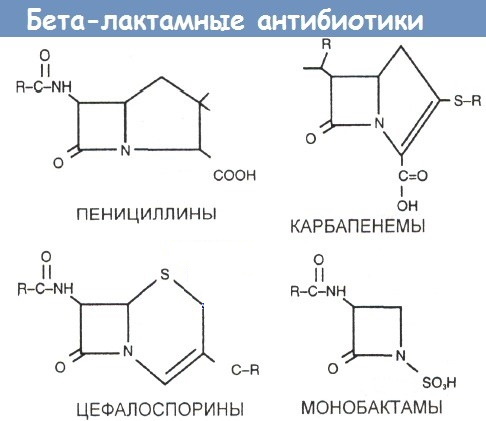
Among the semi-synthetic, the following subgroups are distinguished:
- penicillin-stable penicillins;
- aminopenicillins;
- carboxypenicillins;
- ureidopenicillins;
- inhibitor-protected penicillins.
Cephalosporins are classified into several classes:
- 1st generation.
- 2nd generation.
- III generation.
- IV generation.
Natural penicillins
The main representatives of natural penicillins are benzylpenicillin and phenoxymethylpenicillin.
Benzylpenicillin
Benzylpenicillin is characterized by a powerful bactericidal effect, low toxicity and low cost. Disadvantages include acquired drug resistance in many clinically significant bacteria. Many anaerobes, actinomycetes and all cocci are highly sensitive to benzylpenicillin. It is used parenterally, as it is destroyed when exposed to gastric juice.
Main indications:
- streptococcal infections: tonsillitis, erysipelas, scarlet fever, rheumatism;
- community-acquired pneumonia caused by pneumococcus;
- meningococcal or pneumococcal leptomeningitis;
- sexually transmitted infections (syphilis, gonorrhea);
- anthrax;
- infectious pathology caused by actinomycetes;
- Clostridial infection.
Phenoxymethylpenicillin
The antimicrobial effect of phenoxymethylpenicillin is similar to that of penicillin. But the drug is more resistant to the effects of digestive juices when taken orally.
Main indications:
- streptococcal infectious pathology, not severe;
- infectious pathology of the skin and soft tissues;
- prevention of rheumatism, glomerulonephritis, endocarditis;
- syphilis;
- gonorrhea;
- prevention of complications after minor surgical interventions (removal of tonsils, tooth extraction).
Penicillin-susceptible penicillins
The fundamental difference between penicillinase-stable chemotherapy drugs from other penicillins is resistance to b-lactamases. This subgroup includes oxacillin and cloxacillin.
Oxacillin
In terms of the antimicrobial spectrum, oxacillin is close to natural penicillins, but inferior in activity.

Oxacillin is the drug of choice for the treatment of staphylococcal infectious diseases:
- purulent surgical infections;
- pyelitis and cystitis;
- burns;
- sinusitis.
Oxacillin is not destroyed when administered orally. However, the parenteral route of administration provides a higher concentration of the drug in the blood.
Cloxacillin
The antimicrobial effect of cloxacillin is identical to oxacillin.
Main indications:
- treatment of infectious and inflammatory diseases caused by staphylococci;
- prevention of purulent complications after skin graft transplantation.
Aminopenicillins
The main representatives of aminopenicillins are ampicillin and amoxicillin.
Ampicillin
The antimicrobial activity of ampicillin is the same as that of penicillin. Some gram-negative intestinal bacteria are susceptible to the drug. It is not affected by digestive enzymes, therefore it is administered orally.
Main indications:
- infectious pathology of ENT organs (nasopharyngitis, sinusitis, tonsillitis);
- odontogenic infections;
- bronchopulmonary infectious pathology (pneumonia, bronchitis);
- intestinal infections (not severe);
- meningitis.
Amoxicillin
Due to the short stay in the digestive organs, amoxicillin is ineffective for dysentery. The rest of the antibacterial properties of the drug are similar to ampicillin.
Main indications:
- infectious pathology of the upper respiratory tract, as well as the ear, throat, nose;
- community-acquired pneumonia;
- infectious pathology of the gallbladder and bile ducts;
- urinary tract infections;
- destruction of Helicobacter Pylori (in combination with macrolides and proton pump blockers).
Carboxypenicillins
The most famous chemotherapy drug from the carboxypenicillin subgroup is carbenicillin.
Carbenicillin
The effectiveness of carbenicillin against gram-positive microbes is the same as that of penicillin, but the activity is much less. The spectrum of action of the drug includes the intestinal group of microorganisms and Pseudomonas aeruginosa. Carbenicillin is sensitive to the effects of b-lactamases. Gastric juice destroys the structure of the drug, so it is not prescribed internally.
The use is very limited due to the low antipseudomonal activity.
Ureidopenicillins
The most significant representative of ureidopenicillins is azlocillin.
Azlocillin
Azlocillin is highly active against most gram-negative microorganisms:
- Pseudomonas aeruginosa and other pseudomonads;
- protea;
- Haemophilus influenzae;
- gonococci;
- bacteroids.
The drug is unstable to the action of b-lactamases, therefore clinical use is highly limited.
Inhibitor-protected penicillins
The main mechanism for the development of microbial resistance to b-lactam antibiotics is the synthesis of b-lactamase enzymes. To overcome this mechanism, substances have been created that inactivate b-lactamases.
These include:
- clavulanic acid;
- sulbactams;
- tazobactams.
As a result of the combination of penicillins with the above substances, strong complexes are formed. The use of inhibitor-protected penicillins allows you to expand the spectrum of antibiotic action.
Amoxicillin / clavulanate
Compared to amoxicillin, amoxicillin / clavulanate is more effective against bacteria with acquired resistance, which is due to the synthesis of b-lactamases (Haemophilus influenzae, staphylococci).
The drug does not act on the following microbes:
- Pseudomonas aeruginosa;
- Serratia spp .;
- Acinetobacter spp.
The main indications for the use of amoxicillin / clavulanate are similar to amoxicillin (more often used for chronic inflammatory processes).
Also used for:
- infectious pathology of the skin and soft tissues;
- intra-abdominal infections;
- chemoprophylaxis after surgery.
Ampicillin / sulbactam
The antimicrobial effect of ampicillin / sulbactam is similar to amoxicillin / clavulanate, but it is not used to treat chronic infections.
Main indications:
- bacterial infectious pathology of the throat, trachea, bronchi, lungs, as well as the ear and nose;
- genitourinary infections;
- infectious pathology of the skin and underlying soft tissues;
- postoperative antibiotic prophylaxis.
Amoxicillin / sulbactam
Amoxicillin / sulbactam has a bactericidal effect on a number of microorganisms:
- all cocci (except for oxacillin-resistant ones);
- listeria;
- hemophilic stick;
- anaerobes.
The drug is less active against enterococci and enterobacteria.
Indications for use are:
- infectious pathology of the skin, genitourinary tract, abdominal organs;
- severe pneumonia;
- postoperative prophylaxis in surgery and gynecology.
Ticarcillin / clavulanate
Ticarcillin / clavulanate is indicated for a variety of nosocomial infections (nasocomial infection on mechanical ventilation, abscess pneumonia).
Cephalosporins
The mechanism of action of cephalosporins is similar to penicillins, but they have a more pronounced resistance to b-lactamases.
Generation I cephalosporins
Typical representatives of the 1st generation cephalosporins: cefazolin and cephalexin. These drugs are characterized by a wide spectrum of antimicrobial activity. The predominant effect on gram-positive microorganisms. The main difference between the chemotherapy drugs of this generation is their high anti-staphylococcal activity. Generation I cephalosporins are effective against a number of gram-negative microbes, but are sensitive to the action of b-lactamases.
Main indications:
- sore throats;
- infectious pathology of the skin and subcutaneous fat;
- postoperative prevention of infectious complications.
Generation II cephalosporins
The main representative of the second generation cephalosporins is cefuroxime.
The following microbes are sensitive to the action of the drug:
- gram-negative microbes (Escherichia coli, Klebsiella, Salmonella);
- streptococci;
- staphylococci.
Cefuroxime is used to treat the same infections as the 1st generation cephalosporins.
But due to the effect on gram-negative microorganisms, it is indicated for:
- infectious pathology of the upper respiratory tract;
- infectious pathology of the urinary tract.
Cefaclor is used in the same cases as cefuroxime, except for middle ear infections.
Generation III cephalosporins
III generation cephalosporins are the most popular in the clinic, which is associated with high activity against gram-negative microorganisms (including hospital strains of enterobacteria). Ceftazidime and cefoperazone are used to treat Pseudomonas aeruginosa infections. Cefotaxime and ceftriaxone are active against streptococci and pneumococci, but practically do not affect staphylococci.
Primary Uses for Ceftriaxone and Cefotaxime:
- severe infections of various localization (respiratory organs, musculoskeletal system, intestinal infections);
- biliary tract infections (for cefotaxime);
- bacterial endocarditis and tick-borne borreliosis (for ceftriaxone).
Generation IV cephalosporins
The main representative of IV generation cephalosporins is cefepime. The antimicrobial spectrum of the drug is close to cefotaxime, but it is more active against gram-positive cocci and is more resistant to b-lactamases.
Cefepime is used in cases of severe infections caused by nosocomial polyresistant strains.
Names and prices of drugs
| Drug name | Release form | price, rub. |
| Benzylpenicillin | Vials | 20-100 |
| Phenoxymethylpenicillin | Tablets, syrup | 20-80 |
| Oxacillin | Tablets, vials | 20-50 |
| Ampicillin | Tablets, suspension, vials | 20-50 |
| Amoxicillin | Tablets, capsules, suspension | 50-150 |
| Amoxicillin / clavulanate | Tablets, syrup, vials | 200-300 |
| Ampicillin / sulbactam | Vials | 150-200 |
| Amoxicillin / sulbactam | Vials | 250-300 |
| Cefazolin | Vials | 30-50 |
| Cephalexin | Capsules, suspension | 40-100 |
| Cefuroxime | Vials, tablets, suspension | 100-200 |
| Cefotaxime | Vials | 30-50 |
| Ceftriaxone | Vials | 30-100 |
| Ceftazidime | Vials | 90-110 |
| Cefoperazone | Vials | 100-150 |
| Cefepim | Vials | 100-200 |
B-lactam antibiotics are one of the most numerous groups of chemotherapy drugs. Common features for all representatives are the presence of a b-lactam ring in the structure and a pronounced bactericidal effect. Different drugs differ in the spectrum of antimicrobial activity, which causes differences in indications for use.
Some b-lactams have already lost their relevance due to the development of microbial resistance to them, others are effective for the treatment of even severe, nosocomial infections. Most drugs have low toxicity, and are approved for use during pregnancy and lactation.
Beta-lactams videos
Basic pharmacology of beta-lactams. Part 2:



