Balanoposthitis is a urological pathology, and among the patients in the office of a urologist or dermatovenerologist, one-sixth of men seek help with this problem. The disease is accompanied by inflammation and is more often provoked by two or more pathogens( mixed infection).
Contents
- 1 Balanoposthitis - what is it?
- 1.1 Forms of balanoposthitis
- 2 How can I get a balanoposthitis?
- 3 Symptoms of balanoposthitis in men
- 4 Treatment of balanoposthitis, drugs
- 4.1 Forecast
Balanoposthitis - what is it?
Balanoposthitis is an inflammatory disease that affects the tissues of the inner sheet of the prepuce and the glans penis. These zones come into contact with each other, so most often the infectious process that affected one of them is transmitted to the other.
Less often occurs only postitis, when the foreskin is inflamed, or only balanitis is the inflammation of the penis head.

Various microorganisms can provoke the development of balanoposthitis:
- Bacteria are the most common pathogens, and in most cases, tissues are affected by several of their species. For example, with streptococcal-staphylococcal infection. These two types of bacteria are considered opportunistic, normally live on the skin of a person, but can get on the genitals and under certain conditions begin to multiply uncontrollably. Of pathogenic microbes, balanoposthitis is caused by the gardnerella, pale treponema, chlamydia, gonococcus and others.
Warning! Primary symptom of syphilis - hard chancre - is often located on the head of the penis and can be accompanied by inflammation.
- Fungi are microorganisms of the genus Candida, some of which live in the vagina and urethra in women. Having fallen on the male genitalia, with weakened immunity and other factors, they can provoke inflammation.
- Viruses - they are the least likely cause of balanoposthitis, and fall on the penis in intimate proximity. More often it is genital herpes, which is well established on the mucous membrane of the urethra and the external genitalia.
- Parasitic lesions, for example the simplest microorganisms, are infrequent and prevail in countries with a hot and humid climate - in the tropics.
Forms of balanoposthitis
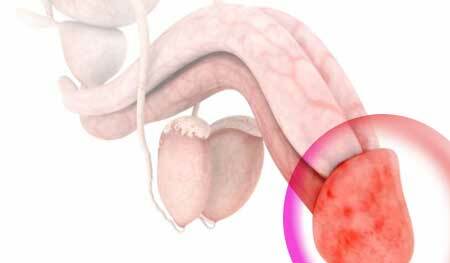
By the nature of the flow of balanoposthitis happens:
- Acute, when the symptoms are pronounced, and the disease progresses quickly;
- Chronic - symptomatology is less intense, the course of the disease is replaced by periods of relapses and remissions.
Acute balanoposthitis in men is more common, its duration is 1-2 weeks. Without the timely treatment of balanoposthitis or in case of illiterate self-treatment without preliminary diagnosis, the disease passes into a chronic form that lasts for months and even years.
There are many forms of balanoposthitis, the most common of them:
- candida;
- herpetic;
- erosive;
- chlamydial;
- circulating;
- purulent;
- anaerobic;
- is ulcerative-pustular;
- gangrenous.
Candidiasis balanoposthitis is one of the forms of candidiasis that develops with a decrease in the body's immune forces and metabolic disorders, for example, in diabetes mellitus. The disease begins with itching, the appearance of a light coating on the surface of the penis, mild hyperemia.
Without treatment, a bacterial infection can join a candidiasis lesion, and the course of the disease passes into a chronic form.
The causative agent of chlamydia balanoposthitis is chlamydia, and pathology acts as a form of urogenital chlamydiosis. It manifests with pain during urination, discharge from the urethra, reddening and a minor focal lesion of the head and foreskin.
Extensive erosions and ulcers occur rarely. Pathology is contagious, and without treatment, inflammation spreads to other organs - the urethra, the epididymis, the prostate gland. A serious complication of chlamydial balanoposthitis is Reiter's syndrome.
This is an autoimmune disorder, aggravating the course of the disease and leading to rash and joint damage and provoking the development of zircinar balanoposthitis.
The herpetic balanoposthitis of is caused by the type II herpes virus, which, after getting into the genital mucosa and then into the bloodstream, may not manifest itself for a long time. If immunity is weakened, the causative agent is activated, forming a rash on the genitalia in the form of painful and itchy watery blisters.
Pathology is sexually transmitted and can affect other organs, in particular the brain.
Genital herpes virus is transmitted by contact with affected genitalia and through biological fluids.
- It is important for both partners to know that if a woman's primary infection occurs during pregnancy, due to the absence of antibodies to the virus in the mother's body, the risk of fetal death or the development of congenital abnormalities of the child's CNS is high.
The erosive form of the balanoposthitis destroys the epithelium and mucosa of the prepuce and the glans penis, which form reddish-pink painful rough sores and erosion.
Over time, the affected tissues develop an infection, purulent areas appear, necrosis along the edge of erosions, and the inguinal lymph nodes increase. The treatment is long, but the scars and scars do not remain after it.
How can I get a balanoposthitis?
The surest way to catch a balanoposthitis is to have unprotected sex with an infection carrier. During sexual intercourse, viruses, bacteria, fungi or protozoan microorganisms can enter the genitalia.
And, some of them, being a part of the normal microflora of the female vagina( for example, staphylococcus), having got on the penis, can begin to multiply actively due to the reduced immunity of a man or other factors.
Therefore, after intimate proximity without a condom, it is important to use antiseptics( Miramistin, Chlorhexidine).The following factors contribute to infection:
- Non-observance of intimate hygiene.
- Random and frequent sex life, not only increases the risk of infection, but also leads to micro-injury and irritation of the mucosa. Pathogens easily settle down on the affected surface, while the integral cutaneous and epithelial cover is a barrier to many microbes.
- Concomitant pathologies that promote the reproduction of microorganisms - diabetes, kidney disease.
- Features of anatomy, for example, an anomaly such as phimosis, in which the foreskin is very narrow and does not bare enough head of the penis. Because of this, a smear accumulates under its sheet, which promotes the reproduction of microbes.
- Exposure to chemicals.
- Cancer of the penis.
- Infectious diseases of the kidneys and urinary tracts - urethritis, pyelonephritis, cystitis, - as well as urolithiasis and hydronephrosis.
Symptoms of balanoposthitis in men
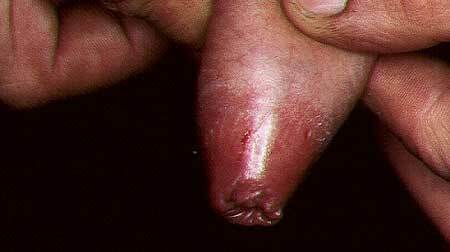
Candidiasis balanoposthitis, photos
With balanoposthitis, the symptoms manifest themselves individually depending on the causative agent of the disease. Most often there is soreness and itching of the epithelium, swelling and reddening of the head of the penis, rarely symptoms are absent for a long time.
In acute balanoposthitis, the symptoms in a man are pronounced, among them:
- Hyperemia and pain;
- Discharge from the urethra;
- Burning sensation when urinating.
It is important to consult a doctor immediately when the first signs appear, otherwise it may develop an erosive-purulent lesion and chronic disease. The chronic form is manifested by minor puffiness, reddening and irritation of the affected area, formation of plaque.
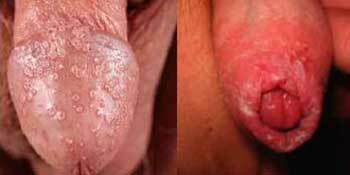
Symptoms of balanoposthitis photo 2
Without timely therapy, soreness increases, and also symptoms of balanoposthitis in men like phimosis, difficulty urinating and erectile dysfunction may develop.
Self-disappearance of signs of an acute form of the disease does not indicate a recovery - the source of inflammation remains in the body and can affect other organs, including the prostate gland.
Treatment of balanoposthitis, preparations
 The treatment regimen for balanoposthitis is determined by a urologist or dermatovenerologist based on the results of tests and examination of the affected area. Therapy involves the use of:
The treatment regimen for balanoposthitis is determined by a urologist or dermatovenerologist based on the results of tests and examination of the affected area. Therapy involves the use of:
- Conservative methods are drugs that affect a particular group of pathogens. Tablets, injections and ointments for the treatment of balanoposthitis appoint depending on the pathogen( antifungal, antiviral, immunostimulating and others).
- Surgical intervention shown when medicines are ineffective. The operation consists in dissection of the foreskin contracted as a result of inflammation or its circumcision.
- Alternative therapy - an auxiliary measure - the use of compresses, trays of herbal decoction and other folk remedies.
In candidiasis balanoposthitis in men, the treatment involves the use of:
- Antifungal drugs - topically Fluconazole, Clotrimazole, Lomexin, Candid, Pimafucin, Tetraborate, ingestion of Diflucan, Flucostate or Itroconazole;
- Laser phaseresis and laser therapy of blood;
- Baths and lotions with decoctions of marigold, barberry, chamomile, cloves.
Gangrenous form is treated with drugs from the group of sulfonamides and antibiotics, topically apply solutions of antiseptics with acidic medium - potassium permanganate, oxygen water, silver nitrate.
When herpetic balanoposthitis is shown:
- Antiviral drugs topically and inwardly( Acyclovir, Famvir, Valaciclovir);
- Immunomodulators and immunostimulants( Lokferon, Tsikloferon, Likopid, Timalin, Viferon, Neovir).
If there is cicatricial phimosis, the foreskin is dissected or cut, and then the affected area is smeared with healing ointments - Panthenol, Levomecol, hormone creams with progesterone, synestrol.
Lotions with 10% solution of carbolic acid are indicated for ulcerative pustular balanoposthitis. Also, 0.1% rivanol solution is used. The erosive form is treated with antibiotics and sulfonamides, bismuth powders.
Forecast
For balanoposthitis in men, treatment should be timely and be prescribed only by a specialist after the diagnosis. In this case, the prognosis is favorable and the risk of complications is practically absent.
After infection with herpetic balanoposthitis, the herpes virus remains in the blood for life, but with a healthy lifestyle, a balanced diet, strengthening of immunity does not appear for many years.
Possible consequences of balanoposthitis:
- Inflammatory lesion of the lymph vessels of the penis and adjacent zones( lymphangitis);
- infection and inflammation of the urinary tract and kidney;
- cicatricial phimosis;
- pronounced pain syndrome, particularly when moving;
- urination during sexual contact;
- erectile dysfunction.

