Content
- Causes of atherosclerosis of the aorta of the heart
- Risk group
- Symptoms
- Complications
- Diagnostics
- Laboratory diagnostics
- Instrumental diagnostics
- Differential diagnosis
- Treatment of aortic atherosclerosis
- Medication
- Surgical
- Diet
- Physical activity for atherosclerosis
- Forecast
- View of aortic atherosclerosis
Aortic atherosclerosis is one thing from common chronic diseases, affecting the main blood vessel. It is characterized by the formation on the inner lining of the cardiac aorta of the so-called "atheromatous plaques" - lipid foci, which are mainly cholesterol deposits.
Causes of atherosclerosis of the aorta of the heart
The disease is a special case of atherosclerosis - damage to the blood vessels that carry blood to the organs from the heart. Such a vessel is the aorta - one of the arteries and the main trunk of the systemic circulation.
The underlying mechanisms of the origin of atherosclerosis are currently not fully deciphered. They speak with confidence only about the immediate cause of the pathology, which causes a chain of tragic changes in the state of the circulatory system.
This reason is the changes in the inner lining of the arteries, which are associated with the deposition of cholesterol and some lipoprotein fractions in the lumen of the vessels. Outwardly, this is expressed in single or multiple deposits of lipid plaques. Gradually, the vessel is deformed, which is explained by the proliferation of connective tissue in its membrane (sclerosis) and the deposition of calcium salts in it (calcification). The lumen of the vessel is narrowed.
Organs and tissues that feed through the affected artery are affected: they experience a lack of blood supply. Oxygen and nutrients can no longer be supplied to them in the proper amount.
Aortic atherosclerosis (what is this pathology and what are the reasons for its development, is considered taking into account the pathogenesis of atherosclerosis) as a whole arises from a violation of lipid and protein metabolism.
Risk group
Factors that increase the likelihood of developing the disease are of great importance. These are age, gender, lifestyle and comorbidities.
The risk group includes people:
- suffering from arterial hypertension;
- with diabetes mellitus, alimentary obesity, hyperlipidemia and other conditions associated with a slowdown in metabolism and impaired lipid metabolism;
- with family heredity burdened by atherosclerosis;
- with an increased level of "bad" cholesterol in the blood;
- experiencing excessive emotional stress;
- smokers;
- with reduced motor activity;
- men from 40-50 years old, women from 55 years old (after menopause);
- elderly.
What matters is irrational nutrition with a predominance of animal fats in the diet.
Symptoms
Atherosclerosis of the aorta (what kind of disease it is, will be discussed later in the article) has various manifestations. First of all, the clinical picture depends on the volume of lipid deposits and the specific localization of the plaque.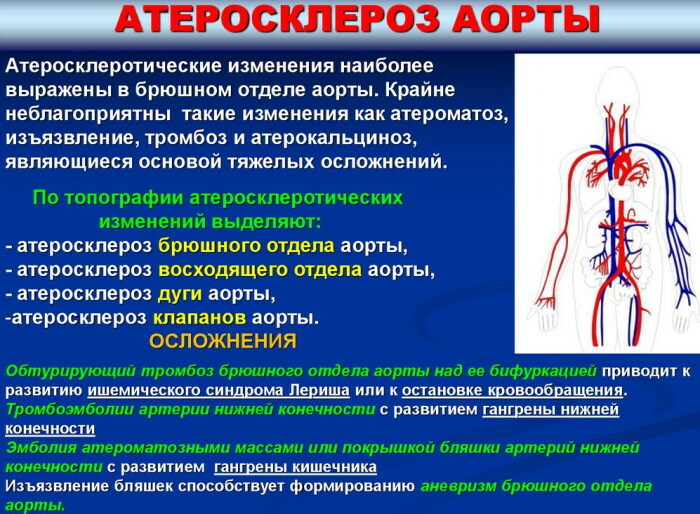
The aorta itself originates from the left ventricle of the heart, taking out blood from it. It goes up, then forms an arc and descends, passing through the chest and abdominal cavity. Then it is divided into smaller arteries.
There are 3 sections of the aorta:
- Ascending. From here originate the right and left coronary arteries, which supply blood to the heart and provide its pumping function.
- Aortic arch, which begins at the level of the junction of the right costal cartilage with the sternum. Through the appropriate arteries, it supplies blood to the head, bronchi, neck and arms.
- Descending department. It runs from level IV of the thoracic vertebra to level IV of the lumbar vertebra. It is divided, in turn, into the chest and abdominal parts. The thoracic aorta is located in the posterior mediastinum. Ventral - on the front surface of the vertebral bodies, slightly to the left of the midline. Nourishes the organs of the chest and peritoneum.
With atherosclerotic lesions of the aorta, the heart and the underlying organs feeding from it suffer.
Atherosclerosis of the ascending aorta often manifests itself only with the appearance of complications.
In this case, the following symptoms are observed:
- severe weakness, possible loss of consciousness;
- pallor of the skin;
- severe chest pain.
When the mouth of the coronary arteries is affected, the symptoms resemble developing heart failure or ischemic heart disease.
The patient experiences:
- shortness of breath, weakness, fatigue;
- cardiopalmus;
- pressing pains in the region of the heart;
- sharp pain in the middle of the chest or on the left side of the chest;
- swelling is possible.
With the defeat of the branches of the aortic arch, signs of insufficient blood supply to the brain or upper limbs predominate:
- feeling weak;
- attacks of night sweats associated with episodes of cerebrovascular accident;
- headache;
- dizziness;
- fainting;
- visual disturbances;
- swelling of the neck and tonsils;
- cold hands.
If the thoracic aorta is affected, the following symptoms may occur:
- prolonged and excruciating pain behind the sternum, radiating to the abdomen, back, ribs, arms or neck;
- headache;
- dysphagia (difficulty swallowing) and hoarseness;

The abdominal part is affected more often and earlier than other parts of the aorta. Symptoms are determined by the location of the plaques and by which part of the body's blood supply is impaired.
There may be the following manifestations:
- belching, heartburn, bloating;
- pallor of the skin of the legs, numbness and coldness of the feet;
- violation of the sensitivity of the legs;
- the formation of trophic ulcers on the lower extremities.
The disease can go unnoticed for a long time, and often symptoms appear already in a critical situation, when life-threatening complications have arisen.
Complications
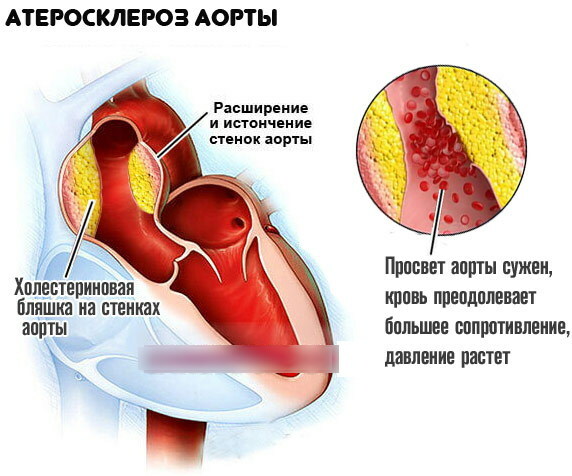
Atherosclerosis changes the strength of the aorta. Its walls are compacted, deformed, and lose elasticity. What this entails becomes clear from an understanding of the principles of the main artery.
Every second, the aorta propels blood, which is pushed out by the heart. In response to an increase in pressure, the tension in the walls of the aorta also increases. Thanks to the elasticity of the connective tissue lining the vessel walls, a healthy aorta is able to withstand these loads.
When the walls are deformed by cholesterol deposits, they become weaker and no longer withstand the pressure of the blood from the inside. There are ruptures that end in internal bleeding.
In addition, atherosclerotic plaques can break down. At the same time, they leave a rough mark on the previously smooth inner lining of the vessel. Platelets easily cling to rough surfaces, forming clumps and blood clots. If a blood clot comes off, it can completely block the artery.
Sometimes the cause of an acute blockage of an artery is the contents of a disintegrated cholesterol plaque; sometimes - a thrombus and a plaque at the same time. In the organs, foci of necrosis are formed (an example of this is myocardial infarction); there is a sharp violation of blood circulation.
In addition to the lack of organ and tissue blood supply, other complications arise.
Dangerous complications include:
- aortic aneurysm;
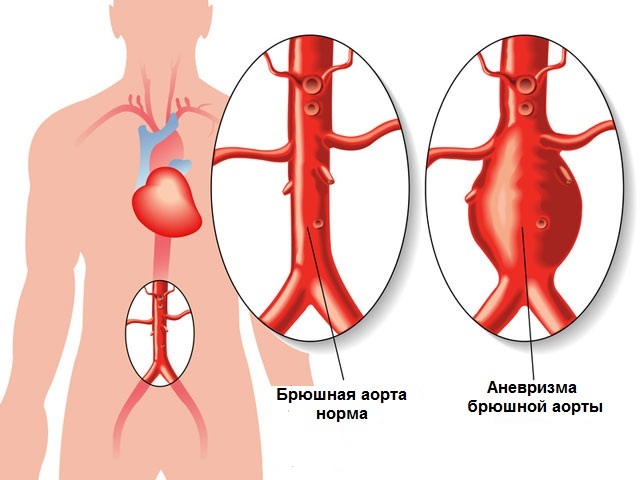
- dissecting hematoma of the aorta;
- aortic thrombosis.
An aneurysm is an enlargement of a part of the aorta caused by weakness or destruction of its wall. Its upper section is more often affected. In this case, the leaflets of the aortic valve expand, and left ventricular failure develops. In addition, an aneurysm threatens with a sudden rupture with bleeding into the retroperitoneal space or into the pleural cavity. Bleeding is often fatal.
With a hematoma, blood accumulates inside the walls of the aorta. Tearing of the inner lining also leads to bleeding, which is manifested by an attack of prolonged and intense pain in the abdominal or cervicothoracic cavity. Collapse develops, blood pressure drops catastrophically.
Thrombosis usually complicates the stenosing course of atherosclerosis of the abdominal aorta, when more than 50% of the vessel lumen is blocked by plaque. Most often, the blockage occurs in the area of the so-called bifurcation of the aorta - the area where it bifurcates into its two terminal branches: the left and right iliac arteries.
An acute disturbance of the blood supply to the legs occurs, which is accompanied by sharp pain, impaired sensitivity and movement. Development of gangrene is possible. The condition is called Leriche syndrome.
Diagnostics
Gradually increasing arterial hypertension is characteristic of atherosclerosis of the aorta. Possible asymmetry of the pulse on the extremities. When listening to the heart, an amplification of the II tone is heard at the listening point of the aortic valves (at the left edge of the sternum at the level of the III intercostal space), above the aorta, above the place of its bifurcation. The left ventricle of the heart is enlarged.
An aneurysm of the abdominal aorta is detected by deep palpation. Subjectively, the patient may feel a strong pulsation in the abdomen.
However, often the disease, especially in the initial stages, is asymptomatic, and is detected when research is carried out for another reason. In other cases, it is necessary to differentiate aortic atherosclerosis from other pathologies. Therefore, for a reliable diagnosis, a number of studies are required.
Laboratory diagnostics
The most valuable is the study of the lipid spectrum of blood, within which a number of analyzes are carried out for the content of fat-like substances in it - lipids. The obtained indicators allow us to assess the risk of developing or having atherosclerosis, as well as associated heart diseases.
The tables indicate the accepted norms of indicators, however, laboratories may have their own reference values.
| Laboratory indicator | Norm | Indicating the risk or presence of atherosclerosis |
| Total cholesterol | 5.1 mmol / L | Exceeding indicators |
| Triglycerides | 1.7 mmol / L | |
| Low density lipoproteins, LDL ("bad" cholesterol) | 4 mmol / l | |
| High density lipoproteins, HDL ("good" cholesterol fraction) | 1.0 mmol / L in men and 1.2 mmol / L in women | Decrease in the indicator. The conclusion is made only taking into account the "bad" cholesterol. |
When diagnosing atherosclerosis, it is important to assess the entire range of laboratory parameters. So, an excess of cholesterol can indicate not only atherosclerosis, but also kidney problems, diabetes mellitus or hypothyroidism. Evaluation of other indicators of the lipid spectrum is important.
Atherosclerosis of the aorta (that this disease is associated with an increased level of LDL, can be seen from the table) is established not only by the indicators of lipoproteins taken separately. What matters is their ratio: HDL to LDL. In men, this proportion is normally 1: 4, in women - 1.2: 4.
HDL is "useful". They have the highest density among lipoproteins, since they contain more protein than fat. These compounds are called "good" cholesterol because they prevent the deposition of "bad" cholesterol in the walls of blood vessels and help to reduce the already forming plaques.
Instrumental diagnostics
For diagnostics, the following studies can be assigned:
- Doppler ultrasound (USDG). Doppler ultrasound is a type of ultrasound, but is used to assess the state of the vessels. The most detailed picture is provided by duplex and triplex scanning. These types of USDG are considered the leading methods for diagnosing vascular disease: scanning allows you to see blood flow in real time, to assess the diameter of the vessel and the structure of the plaque.
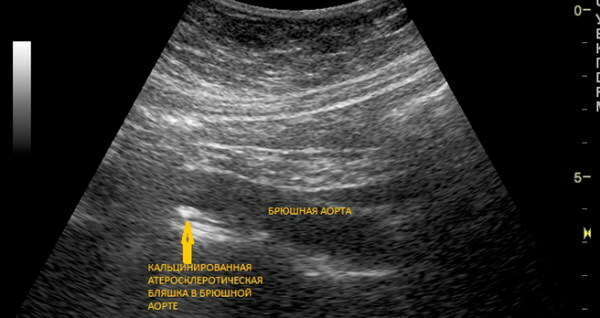
- Angiography, especially contrast arteriography, can detect the exact location and extent of the narrowing of an artery. In some cases, during the study, angioplasty of the narrowed vessel can be performed or a stent placed.
- Magnetic resonance imaging (MRI) makes it possible to identify pathologies of many organs, including the heart and blood vessels.
- Computed tomography (CT) can detect aneurysms. For more informational content, contrast agents can be introduced.
- Electrocardiogram (ECG). The study is usually supplemented by the results of ultrasound of the heart and aorta.
- Transesophageal echocardiography (TEE) is an ultrasound scan of the heart from the esophagus that gives a clearer picture of the aorta.
- Chest X-ray. Allows you to identify the expansion and calcification of the aortic arch.
Differential diagnosis
Atherosclerosis of the main artery must be differentiated from aortitis - inflammatory lesions of its walls. Aortitis is caused by a variety of infections, including bacterial or syphilitic. The pathology is indicated by a persistent increase in the erythrocyte sedimentation rate (ESR).
With aortic hematoma, differentiation with myocardial infarction is required. With a hematoma on the ECG, there are no signs of a heart attack.
The most conclusive sign of atherosclerosis is linear calcifications on the aortic walls, which are visible in lateral projection on radiographs. Although this is the most recent symptom, it is used for differentiation.
Treatment of aortic atherosclerosis
Treatment of atherosclerosis begins with non-drug methods: diet and dosed physical activity. If the desired effect cannot be achieved, drug therapy is added. If complications develop, reconstructive surgery may be required.
Medication
Drug therapy is aimed at lowering the level of "bad" cholesterol and removing it from the body.
Lipid-lowering, that is, lipid-lowering, agents are used:
-
Bile acid sequestrants (cholestyramine). First-line drugs in the treatment of hypercholesterolemia. They bind bile acids in the intestine, which reduces the absorption of cholesterol and increases its excretion. Thus, it is possible to reduce cholesterol up to 40%.

- Fibrates (gemfibrozil, fenofibrate). Reduces triglyceride levels. Effective at normal concentration of total cholesterol with an increase in triglycerides.
- Statins (fluvastatin, simvastatin). They block the enzyme involved in the formation of cholesterol and reduce its content in atherosclerotic plaques. Applied with high cholesterol levels and normal triglyceride concentrations.
- Nicotinamide (enduracin). Aimed at reducing cholesterol (up to 30%) and triglycerides (up to 40%).
Statins and fibrates are contraindicated in case of impaired renal and liver function, pregnancy and lactation. Nicotinic acid is not used for diabetes, gout and gastric ulcer. Sequestrants are not absorbed from the gastrointestinal tract, therefore they have fewer contraindications.
Medicines are selected carefully and in stages, moving from monotherapy with a gradual increase in dose to a combination of drugs.
In many cases, a decrease in the level of atherogenic (leading to the formation of atheroma, that is, plaque) lipids leads to the cessation of the progression of the disease, the reverse development of existing plaques.
Drugs are prescribed to lower blood pressure as the main factor in the development of complications.
Surgical
Atherosclerosis of the aorta (that this disease is dangerous with complications such as rupture of the vessel, described later in the article) requires surgical treatment for large aneurysms. If it is small, the patient is recommended to be monitored with a visit to specialists every six months. If a rapid growth of the aneurysm is noticed, surgical treatment is performed to avoid rupture.
The affected area is replaced with an aortic prosthesis, which is an artificial blood vessel. A less invasive method is the introduction of a special prosthesis using a catheter into the lumen of the vessel. It attaches to healthy areas of the aorta from the inside, above and below the aneurysm. If an aneurysm ruptures, emergency surgery is required.
To remove an atherosclerotic plaque and restore the volume of blood flow, another type of operation is performed: the plaque is removed through an incision in the vessel, and a flap is sewn to the incision site as a patch.
Diet
Dramatically reducing the amount of saturated fat in the diet helps lower the level of "bad" cholesterol in the blood.
It is recommended to reduce or eliminate the following foods from the diet:
- butter;
- egg yolk;
- hard cheeses;
- sausages;
- fat meat;
- fast food.
These foods are high in saturated fatty acids.
The need for fats is satisfied by food rich in polyunsaturated fatty acids:
- fish (salmon, mackerel, herring);
- seafood;
- liquid vegetable oil (flaxseed, olive, sunflower).
The rejection of easily digestible carbohydrates, including bakery products made from premium flour, will bring benefits. It is necessary to reduce body weight if there is excess weight.
To increase blood levels of HDL, a Mediterranean diet is recommended. It allows you to limit the intake of animal fats. Omega-3 supplements may be prescribed in addition to food.
Patients with abdominal aortic aneurysms should avoid foods that cause flatulence. Gas formation in the intestine can provoke an aneurysm rupture.
Physical activity for atherosclerosis
We recommend physical activity commensurate with the age and physical capabilities of the patient. The dosage and form of exercise is recommended by your general practitioner or cardiologist.
Physical activity is generally contraindicated in patients with aortic aneurysm, since there is a risk of rupture.
Forecast
In medicine, the prognosis is characterized as uncertain. The effectiveness of the selected drug treatment and the success of surgical reconstruction of the damaged section of the vessel are of great importance.
Annual preventive examinations allow timely identification of atherosclerotic processes in the aorta of the heart and other vessels. There is no doubt that this reduces the likelihood of developing formidable complications and, ultimately, reduces the mortality rate in cardiovascular diseases.
View of aortic atherosclerosis
Malysheva about aortic atherosclerosis:



