Content
- General concept of genital tuberculosis
- Reasons for the appearance
- Symptoms and Signs
- Development mechanism
- Infected or not
- Transmission routes
- Classification of the disease
- Clinical course
- Tuberculosis of the female genital organs
- In men
- Mycobacterium lesion of the genitourinary system
- Diagnostic methods
- Anamnesis
- Gynecological examination
- Tuberculin tests
- Cultures of genital tract discharge
- Hysterosalpingography
- Laparoscopy
- Histological examination
- Ultrasound
- Other methods
- Treatment principles
- Chemotherapy
- Surgical intervention
- Medication
- Recovery prognosis
- Possible complications
- Preventive actions
- Genital TB statistics
Genital tuberculosis (genital) is an infectious disease caused by the pathogenic mycobacterium Mycobacterium tuberculosis. This pathology has a number of unpleasant symptoms and needs prompt treatment. In the absence of therapy, a number of complications develop. It is extremely difficult to cope with them.
General concept of genital tuberculosis
Genital tuberculosis is not an independent disease. It always develops against the background of a primary infection with Koch's bacillus of the lungs or intestines.
Damage to the organs of the genitourinary system belongs to the type of extrapulmonary tuberculosis. Its incidence is 6.5%.
In patients with such a diagnosis, the inflammatory process spreads to several organs:
- fallopian tubes (they are affected in 90-100% of cases);
- endometrium (less common, in 50-60% of women);
- ovaries (diagnosed in 20-30% of cases);
- cervix (5-15%).
Reasons for the appearance
Mycobacteria enter the reproductive system from the primary focus of infection.
There are several ways of spreading the infection throughout the body:
- with blood flow;
- through the lymphatic system;
- through contact (from closely spaced organs).
The impetus that can cause genital tuberculosis is reduced immunity.
It develops against the background:
- monotonous food;
- unfavorable living conditions;
- frequent stress;
- chronic infectious diseases.
Symptoms and Signs
Most of the patients with this diagnosis are women of reproductive age (20-40 years). In the elderly and adolescents, this disease is relatively rare.
Organ dysfunction occurs due to the negative effect of infection on endometrial tissue, the endocrine system and fallopian tubes.
With a sluggish process, a woman has no painful or unpleasant sensations in the abdomen.
Among the symptoms of a subacute course are called:
- pulling painful sensations in the lower abdomen (in rare cases, doctors take them for emergency conditions);
- rapid fatigue, feeling tired, lethargy, headaches;
- heavy sweating in the morning and at night;
- lack of appetite;
- increased body temperature - up to + 38 ° C (in chronic course, this symptom is absent);
- rapid weight loss.
During the diagnosis, the doctor often identifies:
- adhesions that occur in the pelvic organs;
- obstruction of the fallopian tubes;
- sclerosis of the blood vessels;
- infectious lesion of the urinary tract.
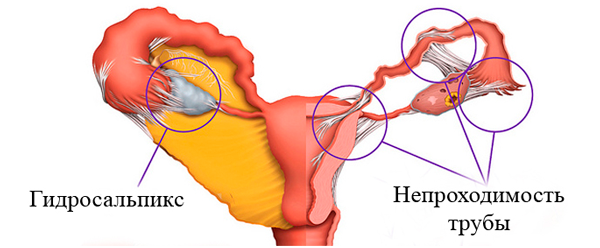
Development mechanism
In most cases of genital tuberculosis, mycobacteria infect the fallopian tubes. This is due to the peculiarities of blood circulation in these organs.
In the human body, the ovarian and uterine arteries, which have numerous bridges (anastomoses), are suitable for the oviduct. This explains the slowed down blood circulation in this organ.
Weak blood flow promotes the settling of mycobacteria on the mucous membrane of the tubes. Over time, pathogens penetrate into the deeper layers of the organ (muscular and serous).
With a prolonged inflammatory process, exudation begins. This term refers to the release of fluid. After some time, the tissues grow and caseous necrosis occurs. As a result of such changes, the passages in the pipes are overgrown, and pus and fluid accumulate in their cavity.
Important information: The clinical picture of the course of fibrocavernous pulmonary tuberculosis
If untreated, the inflammatory process captures neighboring organs:
- in case of damage to the uterus, necrosis and tubercles (tubercles) occur;
- infection on the loops of the intestine and peritoneum leads to the formation of numerous adhesions.
Infected or not
During sexual contact with an infected partner, infection is possible only theoretically. This is explained by the protective function of the epithelium, which lines the surface of the internal organs. These cells are highly resistant to mycobacteria.
Transmission routes
Genital tuberculosis is a secondary disease. It develops against the background of the primary focus.
Classification of the disease
In medicine, this disease is usually classified.
Taking into account the symptoms and histological picture, urogenital tuberculosis has several clinical and morphological forms:
- Chronic. With this course, productive inflammation is observed, there are few symptoms.
- I will subtly. It is characterized by active exudation and tissue proliferation. The clinical picture is well expressed.
- Caseous. With this form, the tissues begin to die off, the course of the disease is severe.
- Completed process. At this stage, the lesions become dense (calcified).
According to the degree of activity, tuberculosis is divided into 3 categories:
- Active. This phase lasts 2 years after infection.
- Fading away (from 2nd to 4th years).
- Inactive. This condition is the consequences of a previous illness.
According to the presence or absence of pathogen bacteria in the analyzes, there are 2 categories of tuberculosis:
- Office (+);
- Office (-).
Clinical course
Patient symptoms often differ. This is due to the localization of the inflammatory process and the size of the infectious lesion.
Tuberculosis of the female genital organs
Among the first signs of the disease are menstrual irregularities caused by hormonal disruption. It can be manifested by excessive discharge or lack of it.
Often, women note an irregular cycle and oligomenorrhea. The latter is a condition in which the interval between periods is 35 days or more.
Depending on the localization of the foci, several pathologies caused by mycobacteria are distinguished:
- salpingitis;
- cervicitis;
- adnexitis;
- metroendometritis;
- damage to the vagina and vulva.
In men
In men with tuberculosis of the genitourinary system, a number of symptoms occur:
- redness and swelling of the genitals;
- ulcers and fistulas on the penis, scrotum, or perineum;
- weakening of potency;
- decrease in the amount of ejaculate;
- unpleasant or painful sensations during orgasm;
- small impurities of blood or pus in the semen.
If the infection has entered the prostate gland and seminal vesicles, then these symptoms are added:
- aching pains localized in the scrotum, lower back and perineum;
- a feeling of heaviness in the rectum;
- frequent constipation.

Mycobacterium lesion of the genitourinary system
With complications, the infection enters the tissue of the peritoneum, the intestinal loops and the bladder. This often causes fistulas to form. They are fistulas, thanks to which the intestines are connected to the external environment.
This pathology is accompanied by several symptoms:
- swelling of the abdominal tissues;
- Difficulty urinating
- constipation and difficulty defecating;
- severe pain.
The examination often reveals papillitis, multiple adhesions.
Diagnostic methods
In most cases, genital TB is difficult to diagnose. This is due to the erased and oligosymptomatic course of the disease. To identify pathology, a complex consisting of laboratory tests, anamnesis and instrumental studies is used.
Anamnesis
At the initial examination, the doctor needs to find out the features of the course of the disease.
For this, the patient must provide some data:
- about the presence of patients with tuberculosis in the family;
- about possible contact with people with such a diagnosis;
- about infection with Koch's bacillus in the past;
- the frequency of diseases of the bronchi and lungs in childhood and adolescence;
- about the presence of chronic inflammation (endometritis, adnexitis).
Important information: Features of the development and course of miliary pulmonary tuberculosis
If the patient has symptoms of urogenital lesions, they must be reported to the doctor.
Gynecological examination
The external manifestation of the disease is observed only with damage to the vulva and vagina. If the inflammatory processes have affected the internal organs of the reproductive system, a superficial examination is uninformative. Palpation is required for diagnosis.
The following signs indicate pathology:
- the appendages are enlarged, their mobility is limited;
- the pipes have a retort-like shape with pronounced swelling;
- the uterus is dense and low mobility;
- in the parametria (adipose tissue, localized behind the uterus), infiltration is often palpated.
Tuberculin tests
A tuberculin test helps to detect infection with Koch's bacillus. During the procedure, the doctor injects 20 TU (tuberculin units) under the mucous membrane of the cervical canal (or subcutaneously).
If the patient is infected with mycobacteria, then after the test, the following reaction occurs:
- the pulse quickens (the number of beats reaches 100 or more times);
- body temperature rises by 0.5 ° C;
- a blood test shows an increase in ESR, an increase in the number of monocytes and stab leukocytes, and a decrease in the number of lymphocytes.
General changes in state occur with the presence of Koch's bacillus in any organ. The local reaction is accompanied by increased pain and swelling in the affected organ.
Cultures of genital tract discharge
To obtain reliable results, triple crops are required. For the purpose of the study, they take an analysis of menstrual blood, vaginal discharge and a wash (or scraping) of the endometrium. An additional diagnostic method is recommended - PCR.
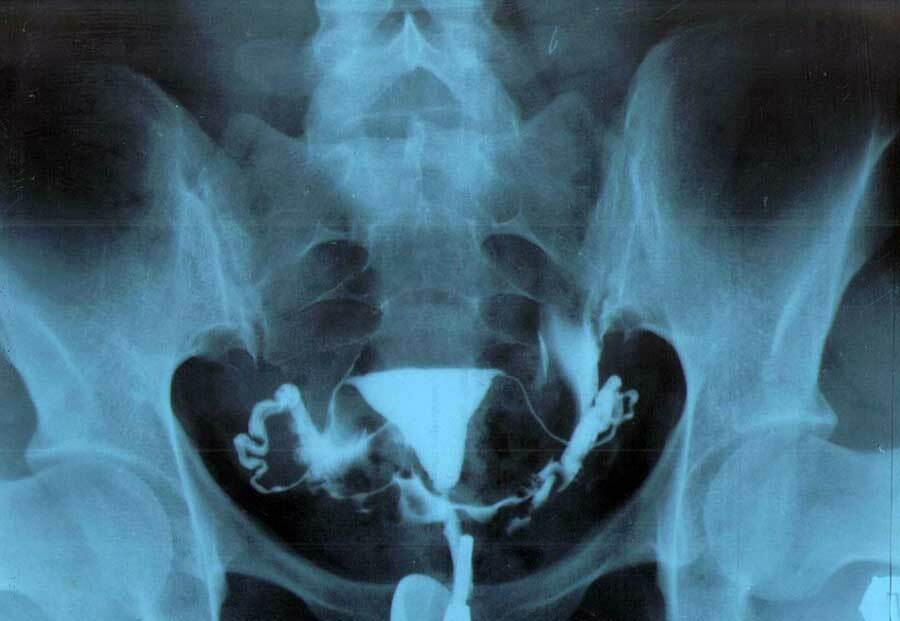
Hysterosalpingography
Hysterosalpingography is understood as an x-ray examination of the tubes and uterus with the introduction of water-soluble contrasts.
The following signs indicate the presence of tuberculosis:
- the uterine cavity is deformed, partially (or completely) overgrown;
- the cervical canal and isthmus have pathological expansion and lengthening;
- peristalsis of the tubes is absent;
- there are pathological shadows on the pelvic organs, indicating caseous foci and calcifications;
- the uterus is displaced to the side;
- the pipe pattern is uneven;
- cyst-like cavities and multiple constrictions are present in the oviducts.
Laparoscopy
Laparoscopy is the most informative diagnostic method.
With its help you can:
- visualize the state of internal organs;
- to collect material for further research;
- restore the patency of the tubes and dissect the adhesions surgically.
Histological examination
Histological examination is the study of samples obtained during curettage of the uterus, biopsy of the organs of the reproductive system and diagnostic laparoscopy.
The signs of the disease in this case are:
- perivascular infiltrates;
- the presence of tubercles with caseous decay and fibrosis;
- large cells of Langhansa (a characteristic feature of tuberculosis).
Ultrasound
Ultrasound does not detect the presence or absence of Koch's rods in the patient's body, however, it provides comprehensive data on the state of the uterus, tubes and ovaries. With the help of this procedure, the size of the organs, the blurring of their contours, the presence of fluid behind the uterus are determined.
Other methods
There are several other studies that are assigned individually:
- culture of urine for mycobacteria (it is taken with a catheter);
- RIA and IFA;
- fluorescence and laser diagnostics;
- X-rays of light;
- X-ray of the digestive system (for some indications).
Treatment principles
The effectiveness of treatment for genital tuberculosis depends on the speed of diagnosis and the correct regimen. The therapy consists of several methods of exposure.
Important information: How is PCR taken for tuberculosis
The doctor prescribes:
- chemotherapy;
- surgical operation (according to strict indications);
- treating symptoms (blocking pain, reducing fever);
- vitamin therapy;
- adherence to a therapeutic diet (a diet rich in vitamins and calories is selected);
- physiotherapy aimed at eliminating adhesions;
- correction of immunity;
- strict adherence to hygiene.

Chemotherapy
Chemotherapy is a course of drugs with bacteriostatic and bactericidal effects. Under the influence of such drugs, Koch's sticks lose their ability to multiply and die.
During the course, the patient takes several medications, because over time, mycobacteria adapt. The therapy can last from 6 to 24 months.
Surgical intervention
The operation is performed only with the following indications:
- the appearance of fistulas;
- ineffectiveness of chemotherapy;
- caseous melting of appendages;
- extensive adhesions that disrupt the work of organs (problems with urination and defecation are often observed).
Medication
Self-administration of medicines is strictly prohibited. The therapy is carried out in a hospital under the strict supervision of a physician. The treatment regimen is selected taking into account the diagnostic data. Small and high doses of drugs can be used.
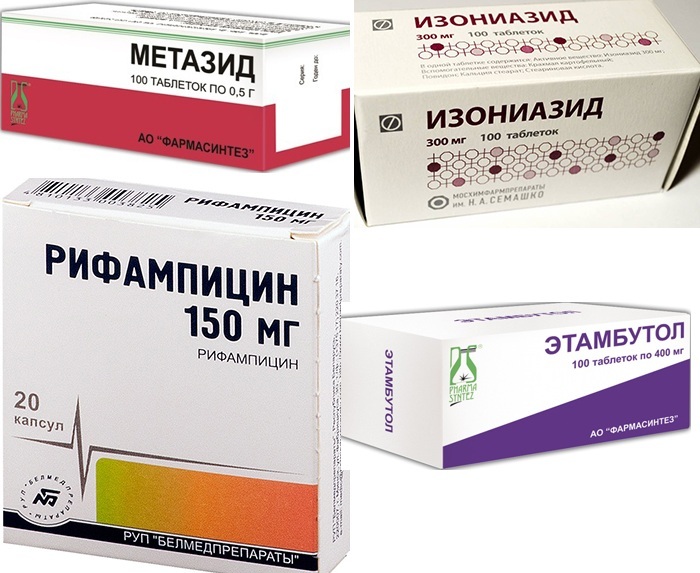
Among the antibacterial drugs are prescribed:
- Metazid;
- Isoniazid;
- Rifampicin;
- Streptomycin;
- Kanamycin;
- Ethambutol.
In some cases, immunostimulants are used:
- Glutoxim;
- Xymedon;
- Galavit.
At high doses of antibacterial drugs, patients often develop drug intoxication.
To relieve such symptoms, they are prescribed:
- Acetylcysteine;
- Rheosorbilactom.
Hepatoprotectors are shown to restore liver function.
The healing processes can be accelerated by:
- Methyluracil;
- aloe-based preparations;
- Glyunat.

Vitamin remedies are called:
- glutamic acid;
- B vitamins;
- ATP (sodium salt).
Recovery prognosis
If therapy is started in a timely manner, the prognosis is favorable. With a late diagnosis, pathology often leads to complications.
In this case, the statistics show:
- relapses of inflammatory phenomena occur in 7-9% of cases;
- reproductive ability remains in 5-7% of women.
Possible complications
A bacterium that enters the female reproductive system is not fatal.
However, the lack of treatment causes numerous complications:
- infertility associated with obstruction of the tubes;
- ectopic pregnancy caused by adhesions;
- spread of infection to neighboring organs (peritoneum, bladder);
- miscarriage and premature birth in case of infection of a pregnant woman.
Preventive actions
Specific prevention includes a set of measures:
- BCG vaccination of infants;
- re-vaccinations of children and adolescents;
- Mantoux reaction for early detection of tuberculosis in children and adolescents;
- regular fluorography in adults.
Non-specific prevention consists in observing several rules:
- Eat a nutritious diet.
- Perform wellness activities.
- Avoid frequent stress and get adequate rest.
- Treat inflammatory diseases in a timely manner.
Genital TB statistics
To assess the risk of developing genital tuberculosis and the consequences of the disease, doctors recommend that patients study statistics.
More than 8 million cases of infection with Koch's bacillus are diagnosed annually in the world. At least 2-3 million patients die from lack of treatment or from complications.
Among women suffering from infertility, genital tuberculosis was diagnosed in 10-25%.
Mycobacterium causes inflammation in the reproductive system in 10-14% of cases.
Mycobacterium tuberculosis is found in 10% of women with cycle disorders.



