Content
- What are atypical lymphocytes and where are they located?
- How do they look?
- Reasons for the appearance
- Viral infections
- Bacterial infections
- Malignant blood disease
- Endocrine Disorders
- What indicators are considered elevated in a child?
- What to do?
- Video about atypical lymphocytes
The main links of the immune system that circulate in the blood and are of great importance in the destruction of pathological microflora and fight chronic infection are lymphocytes. There are 2 types of lymphocytes: T and B.
Each of them produces antibodies, destroys infected cells of the body that can provoke the development of allergies, as well as foreign agents. When it comes to the atypical form, most people have unpleasant associations associated with cancer. In fact, such lymphocytes, detected in a blood test, in most cases have nothing to do with a malignant disease. This is a sign of the presence of an infectious or viral pathology in a child.
What are atypical lymphocytes and where are they located?
Atypical lymphocytes are lymphoid cells that appear against the background of viral infections, often in response to infection with the Epstein-Barr virus, however, can be detected in a blood test and in other diseases of a viral nature in child.
A basic laboratory study that allows you to study the number and shape of erythrocytes, leukocytes, lymphocytes, as well as other important indicators - a general (clinical) blood test. This diagnostic measure is the main way to detect an increase or decrease in the number of lymphocytes, as well as the presence of cells of an atypical shape. An increase in this indicator often occurs in children during illness.
If the doctor established this fact during the diagnosis, then this is one of the important indicators of the presence of infection, viruses, or other pathogenic microflora in the child's body. In other words, alien agents. An increase in the level of lymphocytes and a change in their shape is an indication that they are trying to destroy them. This suggests that the bone marrow begins to produce more white blood cells more intensively, provoking an increase in their number in the plasma.
In the results of laboratory blood tests, atypical mononuclear cells (B-lymphocytes infected with a virus) or plasma cells can be detected. Their presence in peripheral plasma is evidence of an exacerbation of the infectious process, as well as the need for antibody synthesis.
A referral for a diagnostic study is given by the pediatrician after examining the child and talking with the parents.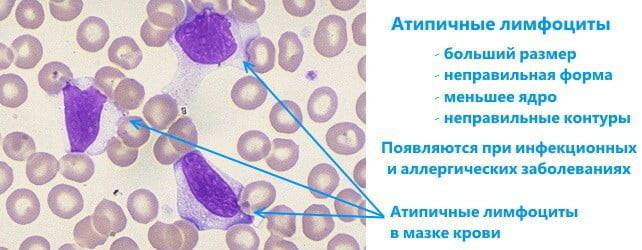
Indications for prescribing a clinical blood test:
- fever lasting more than 5 days, repeated rise in temperature;
- pain in the joints;
- swollen lymph nodes, spleen, or liver;
- the appearance of rashes;
- lack of effect from the therapy;
- severe general condition of the baby.
To obtain the most reliable results, the study is carried out in the morning on an empty stomach.
How do they look?
Atypical lymphocytes in a child's blood test are found in the presence of certain pathologies (viral and infectious, allergies), occurring in an aggravated form. In the plasma, an increase in the number of lymphocytes is observed, as well as the presence of cells with an altered appearance.
Features of atypical cells:
- Modified lymphocytes are enlarged. Cells rarely reach 12 microns. The size of the altered (atypical) is 30 microns and more.
- Ripe cells are rounded. Atypical lymphocytes are often irregular in shape, and their edges are often uneven.
- An ordinary cell has a round or slightly elongated nucleus. An atypical lymphocyte may have the same nucleus, but often it will be elongated, the contours will be uneven, with constrictions or crevices. Sometimes its size can be reduced.
- When staining a smear, which is used to study the number and shape of cells, with typical dyes, atypical cells will acquire a bright color in comparison with unchanged ones. The nucleus will be purple, and the cytoplasm will be blue, dark blue or gray.
- Atypical lymphocytes detected in a patient infected with cytomegalovirus or Epstein-Barr virus are called Downey cells. This is the name of the American doctor-hematologist, who in 1923. discovered them in the process of microscopic examination and described the shape and their properties.
- Another type is Reeder's cells, or amitotic. They are kidney-shaped. The nuclei of such cells have jagged contours, or a constriction in the middle, which divides them into lobes.
- In addition, among the altered lymphocytes, there are Klein-Botkin-Humprecht cells. The name includes the names of three professors who discovered and described the specific cells. In fact, these are not living, full-fledged cells, but their remains circulating in the blood. Due to the fact that they are practically invisible, such lymphocytes are called shadow cells.
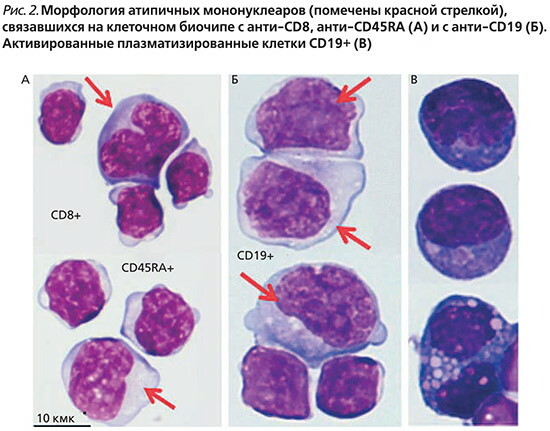
Atypical forms of lymphocytes that can be detected in laboratory research in various pathological processes:
- Small lymphocytes with barely visible cytoplasm and pyknotic nucleus.
- Reeder cells, which are serrated kidney-shaped or bipartite nuclei.
- Lymphocytes with vacuolization in the cytoplasm, in rare cases - in the nucleus.
- Lymphocytes of leukolysis (Botkin-Gumprecht cells) - disturbed during the preparation of the medication, there is a large number in chronic lymphocytic leukemia.
- Naked lymphocytic nuclei.
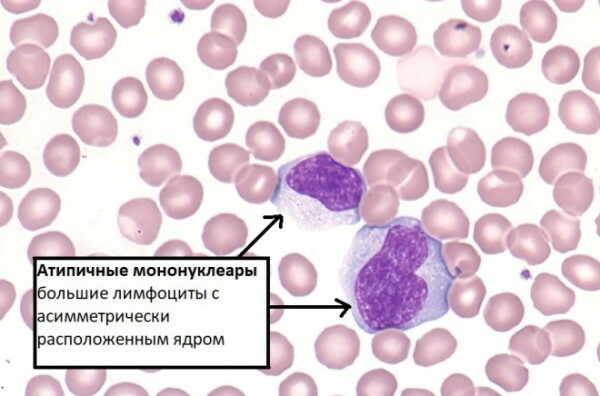
- Atypical mononuclear cells are large cells with abundant basophilic cytoplasm. Often, the basophilic dark peripheral cytoplasm is separated from the paler zone near the nucleus by a thin line border. The nuclei are large, may contain small nucleoli, and in some cases depression is observed. They are visually identical to the nuclei of monocytes. These cells are often found in mononucleosis of an infectious nature, but they can also occur in other infections provoked by viruses.
- Plasmatized lymphocytes are broad-plasma cells with a tympanic nucleus and cytoplasm of intense blue color. Detected in laboratory research in the presence of viral infections.
Reasons for the appearance
Atypical lymphocytes in a child's blood test are developed cells that did not have time to fully form against the background of the disease and begin to fight against the causative agent of the pathology or allergen. As a result, the number of altered lymphocytes in the blood increases.
At the same time, despite the modified appearance, they continue to perform their functions. When pathology develops in a child's body, he needs protection, so the immune system begins to intensively produce lymphocytes in order to cope with the pathological microflora.
Viral infections
Lymphocytes are cells that are the backbone of the immune system in the fight against viruses and bacteria. They produce immunoglobulins (specific antibodies), which, by binding to pathogenic microorganisms, prevent them from entering the cells of the body.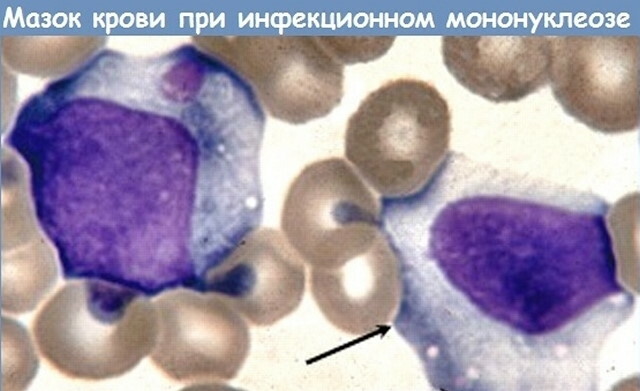
In addition to changing the number of lymphocytes, infectious diseases of a viral nature stimulate the formation atypical cells (virocytes) with a basophilic cytoplasm, a varied shape, a modified structure kernels. They are present in the blood in small numbers (less than 10%) with any infection provoked by viruses. An increased concentration of modified cells (more than 10%) is a sign of infectious mononucleosis.
- Acute viral infections. The most common reason for the formation of atypical cells in children is the following infectious pathologies: rubella, chickenpox, measles. In most cases, the number of such lymphocytes is moderate; as the symptoms are eliminated, the indicators return to normal.
- Infectious mononucleosis. A specific infection of a viral nature in children. Development is provoked by the Epstein-Barr virus. With this pathology, the presence of atypical lymphocytes is more persistent, in analyzes they can be detected over several weeks or even months.
Bacterial infections
The formation of atypical lymphocytes in children can be provoked by an extremely acute bacterial infection - whooping cough. In most cases, modified cells arise against a background of minor lymphocytosis, while almost always relative, accompanied by a general reduction in the number of leukocytes.
Malignant blood disease
The most serious reason for the formation of modified lymphocytes in children is lymph and myeloproliferative pathologies. This disorder is caused by malignant changes in blood cells in the bone marrow and proliferation of tumor clones of lymphatic tissue.
Endocrine Disorders
Pathologies of the organs of the endocrine system can provoke the appearance of modified lymphocytes. The reliable principle of operation of this phenomenon has not yet been fully studied. Moderate numbers of atypical lymphocytes are often associated with increased levels of eosinophils in the blood. The most common cause in children is congenital dysfunctions of the gonads. The formation of altered cells quickly stops after hormone replacement therapy.
Non-infectious factors that provoke an increase in the number of modified lymphocytes include immune reactions, including allergic and autoimmune. So, often such violations are observed as a result of intolerance reactions - allergies, especially in the case of delayed reactions. Often, if the immune system is strained as a result of specific sensitivity and during the vaccination period, the number of lymphocytes, as well as the formation of modified cells, increases.
In addition, this result is characteristic of reactions to stressful situations and autoimmune processes, when the response to inflammation is formed in the tissues of the body. The immune system perceives such manifestations as foreign. Often, in this way, the immune system reacts to endocrine disorders of the body as a result of hyperthyroidism, as well as therapy with certain specific medications.
What indicators are considered elevated in a child?
Atypical lymphocytes in a child's blood test can be detected even in the absence of any diseases within no more than 10%. Exceeding this indicator indicates the presence of pathogenic microflora in the body. In this case, it is important to determine the total level of lymphocytes.
The norms of this indicator in the blood of a child depend on his age. In infants, their number is increased. Gradually, as they grow older, this figure decreases. From the moment of birth, the human immune system begins to form in stages.
In the first year after birth, the maximum level of lymphocytes in the blood is recorded. Upon reaching 5-6 years, the level of these cells is reduced to minimum levels, and such fluctuations are considered the norm.
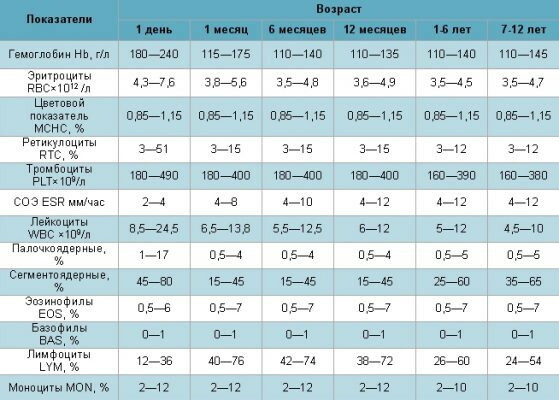
There is a special table that is designed to help pediatricians and parents navigate in order to determine when indicators are considered normal, and when they are a sign of pathology.
Norms of the level of lymphocytes in the blood, taking into account the age of the child:
| Child's age | Normal indicators |
| Newborn | 15-36 |
| 1-7 days of life | 21-55 |
| 1 month | 45-75 |
| Up to 6 months | 55-70 |
| Up to 1 year | 50-70 |
| Up to 2 years | 30-60 |
| Up to 6 years old | 32-55 |
| Up to 12 years old and older | 30-50 |
 According to the table, it can be argued that the indicators that are the norm for a newborn, or a child under 1 year, for a baby who has reached the age of 6 years, there will be a pronounced deviation, which indicates the development diseases. Any excess of the above norms in the results of a clinical blood test, as well as the presence of modified lymphocytes, is a sign of the presence of foreign agents in the body.
According to the table, it can be argued that the indicators that are the norm for a newborn, or a child under 1 year, for a baby who has reached the age of 6 years, there will be a pronounced deviation, which indicates the development diseases. Any excess of the above norms in the results of a clinical blood test, as well as the presence of modified lymphocytes, is a sign of the presence of foreign agents in the body.
What to do?
Atypical lymphocytes in a child's blood test indicate that the immune system has activated the production of antibodies in order to resist the pathology developing in the body. If this violation is detected against the background of an illness or infection, the child is under the supervision of a pediatrician, who prescribes the delivery of control clinical blood tests.
In the case when the symptomatology has decreased, or has completely passed, and the number of atypical lymphocytes does not decrease, the child is shown consultation with a hematologist, who will conduct a deeper study in order to identify all possible causes of the appearance of altered cells in the blood.
If standard studies and manipulations did not reveal the cause, the child may be prescribed additional diagnostic methods: PCR test for detection of latent infections, assessment of the immunogram, as well as bone marrow puncture with subsequent examination of the biomaterial (cytological and histological analysis).
Diagnostic measures are selected individually in each specific case, depending on the clinical picture of the development of pathology in the child. If indicated, a chest x-ray, MRI or CT scan of certain parts of the body or organs, an ultrasound of the abdominal cavity may be prescribed. An accurate diagnosis is determined by the results of laboratory tests and data obtained from instrumental and other studies. Treatment tactics are developed depending on the diagnosed disease.
If the child has a fever, the doctor may prescribe antipyretic medications. Also, according to indications, they can carry out anti-inflammatory or antiviral therapy with special drugs.
If the cause of an increase in the level of lymphocytes, as well as the formation of altered cells, is a neoplasm, further treatment tactics are determined by the specialist depending on the form of the tumor and its activity development. In this situation, chemotherapy or bone marrow transplant may be used.
The presence of atypical lymphocytes indicates that the immune system is working to its limit. If you have symptoms of viral or infectious diseases in a child, you should contact a pediatrician, who will conduct a comprehensive examination to find out the reason for the presence in the blood test of modified cells. Self-medication is strongly discouraged.
Video about atypical lymphocytes
Development of T-cells / T-lymphocytes:



